Prior Authorization That Never Delays Patient Care
HIPAA Compliant
600+ Payer Relationships
All Specialties Covered
<4hr Average Turnaround
The Biggest Administrative Burden in Healthcare — Finally Off Your Plate
Horizon Revenue Group operates a dedicated prior authorization team with deep payer intelligence across 600+ commercial, Medicare Advantage, and Medicaid plans. We know each payer's clinical criteria, submission portals, turnaround expectations, and escalation pathways — and we manage every authorization from initial request through approval, renewal, and appeal so nothing falls through the cracks.
● Initial Auth Requests
● Auth Renewals & Extensions
● Peer-to-Peer Reviews
● Expedited & Urgent Auths

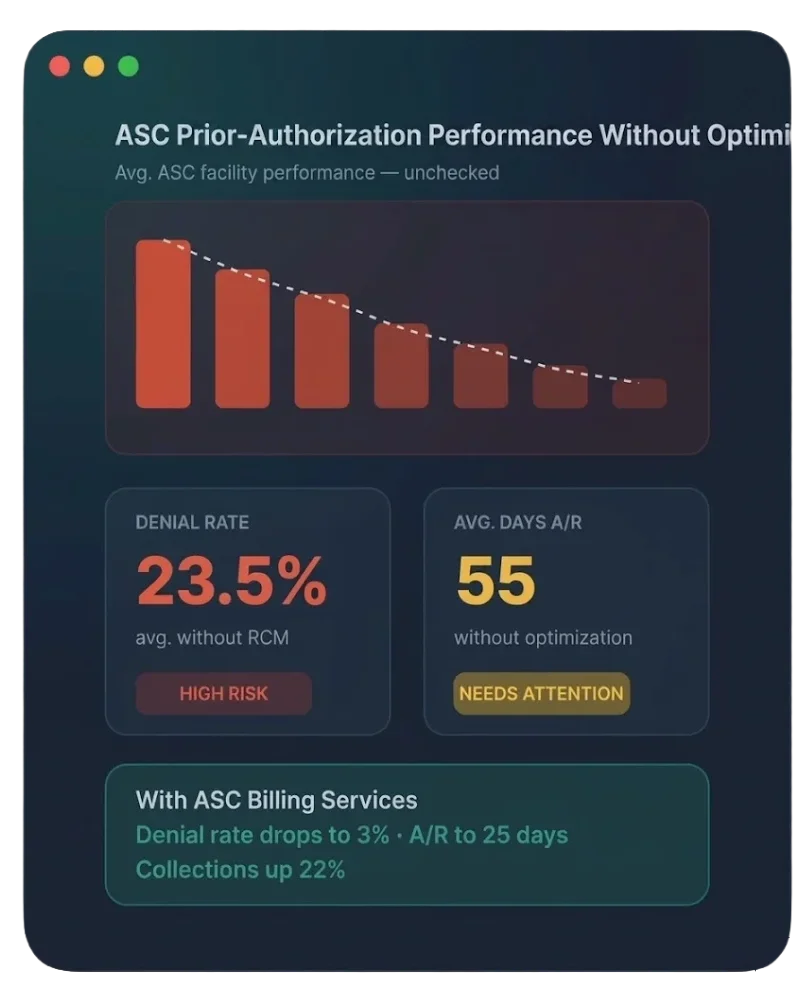
Why Prior Auth Failures Cost Practices Millions Annually
Authorization Denials Triggering Claim Denials
When a prior authorization is denied, rejected, or not obtained at all, every subsequent claim for that service is automatically denied — often without any alert to your billing team until the EOB arrives weeks later.
Clinical Staff Buried in Administrative Work
AMA studies report physicians spend nearly 3 hours daily on prior auth alone. Nurses and medical assistants spend even more — pulling them away from direct patient care and driving staff burnout in already stretched practices.
Expired Authorizations & Retroactive Denials
Authorizations have expiration dates. Services rendered after an auth expires — or before renewal is confirmed — generate retroactive denials that are significantly harder to appeal and often result in full write-offs.
Payer-Specific Rule Complexity & Constant Change
Each payer maintains different clinical criteria, documentation requirements, submission portals, and turnaround timelines — and updates them frequently. Keeping up without a dedicated team leads to systematic submission errors and avoidable denials.
Complete Authorization Coverage — Every Payer. Every Specialty.
Initial Authorization Submission
Complete intake, medical record compilation, letter of medical necessity drafting, and electronic or phone-based submission to the payer — with same-day processing for standard requests and immediate escalation pathways for urgent or time-sensitive cases.
Urgent & Expedited Authorization
Dedicated expedited authorization protocols for urgent surgical cases, emergency admissions, time-sensitive oncology treatments, and same-day procedures — including direct escalation to payer medical directors and 24/7 on-call authorization support for your facility.
Specialty Drug & Infusion Authorization
Expert authorization management for high-cost specialty pharmaceuticals, biologics, infusion therapies, and chemotherapy regimens — including step therapy compliance, clinical exception documentation, manufacturer hub coordination, and prior auth through specialty pharmacy networks.
Auth Denial Appeals & Peer-to-Peer Reviews
Systematic appeal of every denied authorization — including written clinical appeals with evidence-based literature, coordination of physician peer-to-peer reviews with payer medical directors, and external independent review organization (IRO) submissions when required by state law.
Authorization Renewals & Extensions
Proactive monitoring of every active authorization's expiration date — with renewal submissions initiated 30 days in advance, extension requests when clinical timelines shift, and real-time alerts to your scheduling team so services are never rendered against an expired auth.
Real-Time Authorization Status Tracking
A centralized authorization tracking system gives your scheduling, clinical, and billing teams instant visibility into every pending, approved, denied, and expiring authorization — eliminating the phone-tag chaos of manual status checking and ensuring your OR and appointment schedule is always auth-ready.
Medical Necessity Documentation
Clinician-reviewed letters of medical necessity tailored to each payer's specific clinical criteria and evidence-based coverage policies — written to maximize first-pass approval rates by addressing every required element before the payer ever asks for additional information.
Retro-Authorization & Retroactive Appeals
When services are rendered without authorization due to emergency circumstances or payer processing failures, Horizon pursues retroactive authorization requests and payer appeals — recovering reimbursement for services that most practices simply write off as uncollectible.
Authorization Analytics & Denial Reporting
Detailed reporting on authorization approval rates by payer and procedure, denial root-cause analysis, average turnaround benchmarking, and revenue-at-risk tracking — giving your leadership team the intelligence to negotiate contracts and improve payer relationships proactively.
— Key Benefits
What Horizon Authorization Management Delivers
No More Authorization-Related Claim Denials
Every billable service is confirmed auth-approved before it's rendered. Our proactive tracking system eliminates the scenario where your billing team discovers an auth error only when the claim comes back denied weeks later.
Your Clinical Team Focused on Patients — Not Paperwork
When Horizon manages your authorization workflow, physicians, nurses, and medical assistants are completely freed from payer phone queues, portal logins, and documentation requests — returning hours of patient-care capacity every single day.
Faster Treatment Delivery for Your Patients
Sub-4-hour average turnaround means treatments, procedures, and referrals move forward without delay — improving patient outcomes, satisfaction scores, and your practice's reputation for getting things done.
Higher Appeal Win Rates When Denials Happen
Our 85% appeal win rate on denied authorizations means your practice recovers revenue that in-house teams typically abandon. We pursue every denial with payer-specific clinical evidence and physician advocate coordination.
A Proven Workflow That Gets Approvals — Fast
Authorization Intelligence That In-House Teams Can Never Replicate
600+ Payer-Specific Playbooks
We maintain detailed, continuously updated workflow guides for every major payer — covering clinical criteria, required documentation, submission portals, turnaround SLAs, and escalation contacts — so no request is ever submitted blindly.
Dedicated Clinical Appeals Writers
Our appeals team includes former utilization management nurses and clinical documentation specialists who write payer-specific appeals grounded in peer-reviewed evidence — achieving an 85% reversal rate on denied authorizations.
EHR-Integrated Authorization Workflow
Horizon integrates directly with Epic, Athenahealth, eClinicalWorks, and other leading EHR systems — receiving authorization orders automatically, updating approval status in real time, and triggering billing workflow upon auth confirmation.
Proactive Policy Change Monitoring
Payer medical policies change constantly. Our compliance team monitors every major payer's utilization management policy updates and immediately adjusts your submission workflows — so you're never caught submitting a request that was approved last month but denied this month.

— FAQs
Prior Authorization Questions — Answered
Clear, data-backed answers to the financial questions your CFO cares about most.
— Start Today
Ready to Eliminate Authorization Delays & Denials?
Get a free prior authorization workflow audit and find out exactly how many hours your practice is losing — and how much revenue is at risk from auth gaps and denials.
