— ABA Therapy Billing & Revenue Cycle Management
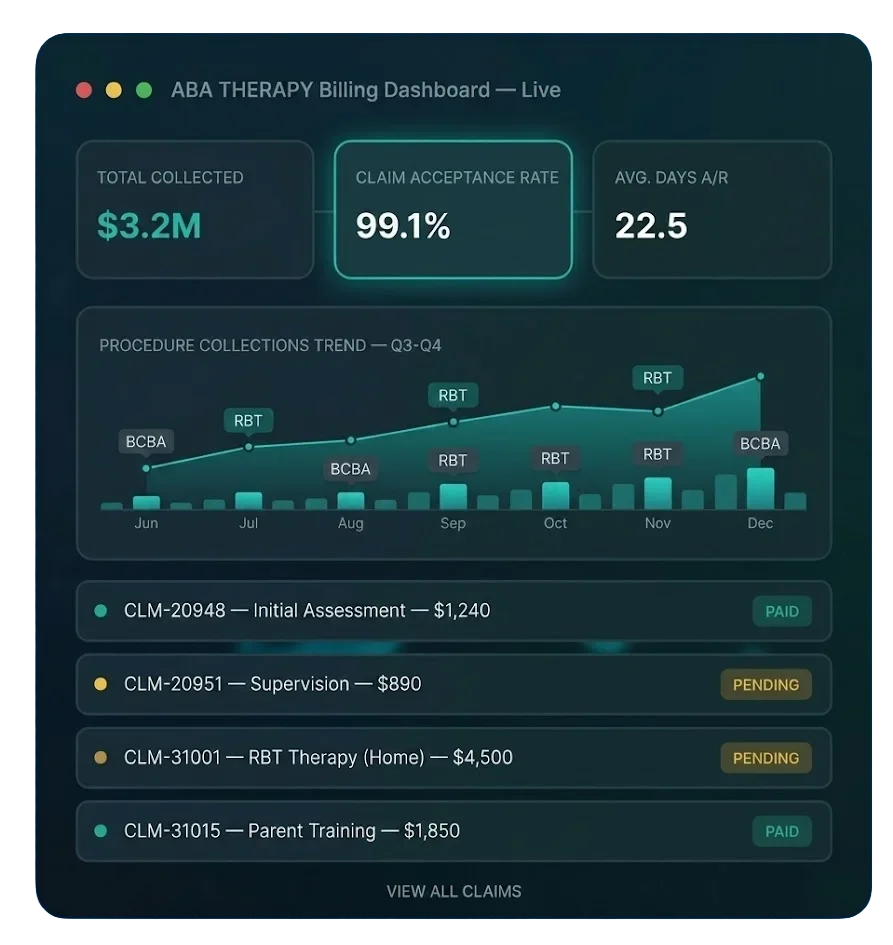
ABA Billing That Recovers Every Therapy Hour
HIPAA Compliant
ABA-Certified Billing Experts
300+ ABA Providers Served
Daily Note Submission
The Most Authorization-Heavy Billing in Behavioral Healthcare — Mastered
Horizon Revenue Group's ABA billing specialists bring deep expertise in Applied Behavior Analysis CPT coding, insurance authorization management for multi-hour daily services, Medicaid waiver billing, RBT and BCBA credentialing, and payer-specific ABA coverage policies. We don't apply generic behavioral health billing logic to ABA claims — we build revenue cycles engineered for the operational realities of high-frequency ABA service delivery.
● CPT 97151–97158 Experts
● Authorization Management
● Medicaid ABA Billing
● BCBA / RBT Credentialing

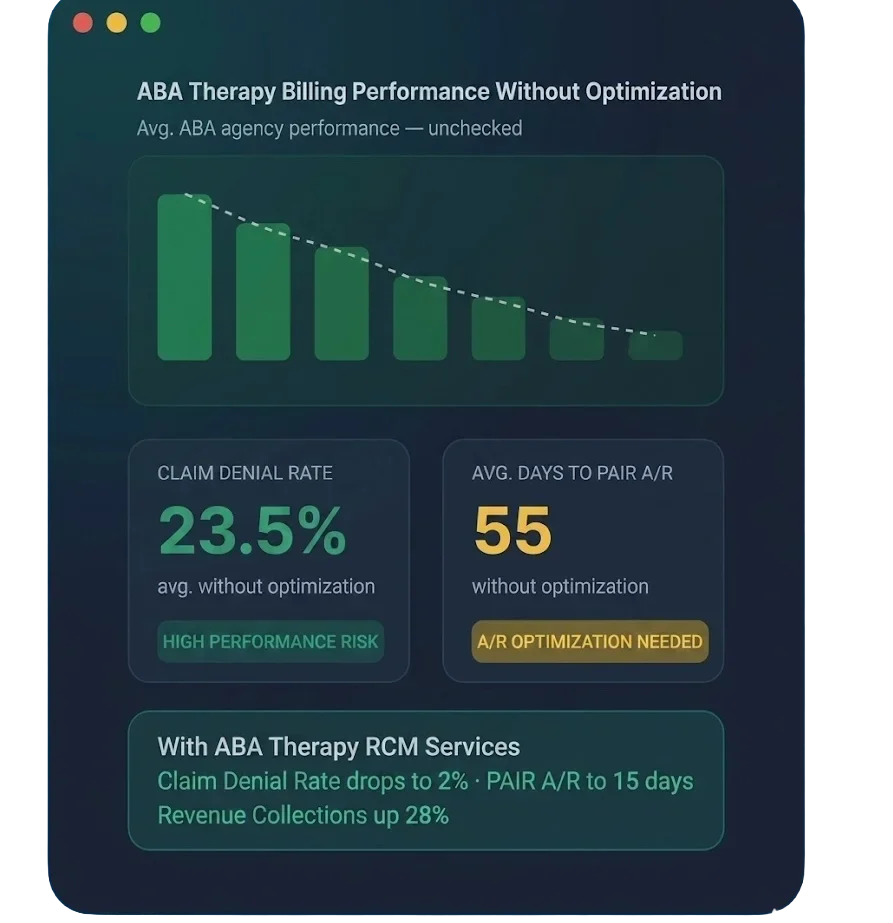
Why ABA Practices Lose More Revenue Than Any Other Specialty
Authorization Expiration & Lapse Denials
ABA services require continuous, rolling authorizations that can cover 20–40 hours of therapy per week per client. A single missed renewal can result in weeks of unbillable sessions and tens of thousands in lost revenue.
Unit-Based Billing Errors & Overcounting
ABA CPT codes bill in 15-minute units. Miscounted units, overlapping service times across technicians, and concurrent session documentation errors trigger costly recoupment audits and retroactive denials.
BCBA Supervision Ratio Documentation Failures
Payers require documented BCBA oversight of RBT-delivered sessions. Missing supervision logs, incorrect credentialing of supervisors, or ratio violations result in blanket denial of all supervised therapy units.
Medicaid ABA Rule Complexity
Each state Medicaid program applies unique ABA coverage rules, billing codes, prior authorization requirements, and BCBA credentialing standards — creating a compliance minefield for multi-state ABA organizations.
Complete ABA Billing Coverage — Zero Gaps
ABA Prior Authorization Management
End-to-end authorization intake, submission, tracking, and renewal for every active ABA client — including initial assessment authorizations (97151), treatment plan renewals, and multi-payer concurrent coverage management so therapy never stops due to auth gaps.
ABA CPT Coding (97151–97158)
Certified ABA billing specialists apply precise unit-based coding across the full ABA CPT range — 97151 (assessment), 97152 (observation), 97153 (discrete trial), 97154 (group), 97155 (BCBA modification), 97156 (family training), 97157 (multi-family), and 97158 (group with BCBA) — maximizing every billable unit.
Medicaid ABA Billing & Waiver Programs
State-by-state Medicaid ABA billing expertise — including Home and Community-Based Services (HCBS) waivers, EPSDT ABA mandates, Medicaid fee schedule compliance, and prior authorization through state Medicaid portals — for providers operating across multiple states.
Daily Session Note & Claim Submission
Automated daily claim generation tied directly to your session notes and ABA data system — with unit verification, overlap detection, and supervisor ratio confirmation before every claim is submitted, keeping your billing current and your cash flow predictable.
ABA Denial Management & Appeals
Rapid review of all ABA claim denials — including medical necessity appeals with assessment reports and treatment plans, BCBA supervision documentation appeals, auth-related denials with clinical support, and Medicaid recoupment defense — with payer-specific escalation protocols.
A/R Follow-Up & Aged Claim Recovery
Systematic follow-up across all outstanding ABA claims — including targeted recovery of aged balances 30–120+ days, coordination between primary insurance and secondary Medicaid coverage, and co-insurance resolution for families with dual coverage.
BCBA & RBT Provider Credentialing
Full credentialing and re-credentialing of BCBAs, BCaBAs, and RBTs with commercial insurers and state Medicaid programs — including CAQH profile management, payer enrollment, NPI management, and supervision agreement documentation for each provider tier.
Family Billing & Patient Responsibility
Clear, family-friendly billing statements that break down session-level charges, insurance payments, and remaining balances — with flexible payment plans, online payment portals, and empathetic communication strategies tailored for families managing high-frequency ABA services.
ABA Analytics & Compliance Reporting
Real-time dashboards with authorized vs. delivered hours tracking, CPT code utilization by therapist, payer reimbursement rate benchmarking, authorization utilization alerts, and Medicaid compliance reporting — giving your leadership team complete revenue visibility.
— Key Benefits
Measurable Outcomes for ABA Therapy Providers
Zero Therapy Hours Lost to Auth Lapses
Our proactive authorization management system tracks every client's active auth window, triggers renewals 30 days in advance, and coordinates with payers to ensure continuous coverage — so your therapists never have to pause services due to a billing oversight.
Every Unit Billed, Every Unit Collected
ABA-specialized coders verify session notes against authorized units, catch underbilling and overcounting before submission, and ensure every 15-minute unit of therapy delivered is converted into a clean, payable claim.
BCBA Supervision Compliance Protected
We maintain complete supervision documentation for every RBT-delivered session — protecting your practice from retrospective audits, recoupment demands, and the compliance risk that comes with incomplete BCBA oversight records.
Multi-State Medicaid Billing Managed
Whether you operate in one state or ten, Horizon tracks each state's ABA-specific Medicaid billing rules, CPT code sets, authorization portals, and BCBA credentialing requirements — so your expansion never creates a compliance blind spot.
A Structured Workflow Built for High-Frequency ABA Service Delivery
ABA Billing Depth That No General Medical Biller Can Match
ABA-Credentialed Billing Specialists
Our billing team holds AAPC and specialty ABA billing credentials — with hands-on experience coding 97151–97158, managing Medicaid ABA programs across multiple states, and navigating commercial ABA carve-out policies.
Integrated Auth Tracking & Utilization Alerts
Our authorization management system monitors every client's approved hours in real time — alerting your team when utilization thresholds trigger renewal requirements, preventing the auth lapses that cost ABA practices thousands per week.
ABA Practice Management System Integrations
We integrate directly with leading ABA data collection and practice management systems — including CentralReach, Catalyst, and Rethink — enabling seamless daily billing without manual data re-entry or session reconciliation errors.
Medicaid Audit Defense & Recoupment Protection
If your practice faces a Medicaid audit or recoupment demand, Horizon's compliance team prepares your documentation response, coordinates legal support, and advocates on your behalf — protecting the revenue you've already earned.

— FAQs
ABA Therapy Billing Questions — Answered
Clear, data-backed answers to the financial questions your CFO cares about most.
— Start Today
Ready to Maximize Your ABA Practice Revenue?
Get a free, no-obligation ABA revenue audit and discover exactly how many therapy hours your practice could be recovering.
