— End-to-End A/R Recovery Solutions
Recover Revenue You’ve Already Earned
Horizon Revenue Group specializes in aggressive and strategic A/R recovery — turning unpaid claims into collected revenue. We identify aging balances, resolve denials, and pursue every outstanding dollar to improve your cash flow and reduce write-offs.
HIPAA Compliant
Certified Billers
Full Cycle Coverage
500+ Practices Served
— What We Do
Your Outstanding Revenue — Recovered & Optimized
Accounts Receivable is where lost revenue hides. Horizon Revenue Group takes full control of your aging A/R — from identifying unpaid and underpaid claims to aggressive follow-ups and final payment resolution — so your practice stops losing money and starts collecting it.
Our A/R specialists bring deep expertise across cardiology, internal medicine, dermatology, mental health, pediatrics, and more. We don’t just follow up — we strategically analyze payer behavior, fix root causes, and recover revenue that would otherwise be written off.
● Aging A/R Analysis
● Denial Resolution & Appeals
● Payer Escalation Strategies
● Real-Time A/R Performance
— Core Services
Turn Outstanding Balances Into Collected Revenue
We focus on what matters most — recovering the money your practice has already earned but hasn’t received. Our A/R recovery process targets aging claims, eliminates bottlenecks, and accelerates cash flow so you can stay financially strong.
Aging Accounts & Uncollected Revenue
Old and neglected claims often go untouched, leading to massive revenue loss. We identify, prioritize, and aggressively work aging A/R to recover payments before they turn into write-offs.
Denied & Stalled Claims
Unresolved denials and stalled claims sit in your system draining revenue. Our team reworks, appeals, and follows through until every claim reaches a final resolution.
Underpayments & Missed Revenue
Payers often underpay claims without notice. We audit payments, identify discrepancies, and recover the revenue you rightfully deserve.
Slow Follow-Ups & Poor A/R Velocity
Delays in follow-ups increase days in A/R and hurt cash flow. We implement fast, consistent follow-up cycles to accelerate reimbursements.

— Services Included
Complete A/R Recovery Coverage — No Revenue Left Behind
A focused A/R recovery system designed to track, pursue, and collect every outstanding dollar — with zero gaps in follow-up and full visibility into your receivables.
A/R Audit & Aging Analysis
We perform a deep audit of your accounts receivable, segmenting aging balances by payer, denial reason, and dollar value — so recovery efforts are always prioritized for maximum impact.
Denial Resolution & Appeals
Every denied claim is analyzed, corrected, and re-submitted with a targeted appeal strategy. We focus on fast turnaround and high overturn rates.
Insurance Follow-Ups
Consistent and aggressive payer follow-ups ensure no claim sits idle. We maintain strict follow-up cycles until payment is received or fully resolved.
Underpayment Recovery
We identify underpaid claims through payment audits and recover the missing revenue from payers based on contract rates and fee schedules.
Aging A/R Collections
Old claims require special attention. Our age-based escalation strategy targets 30, 60, 90+ day balances to recover revenue before write-offs occu
Payer Escalation & Dispute Handling
Complex claims are escalated directly to payer representatives with documented follow-ups and dispute tracking to ensure resolution.
Patient Balance Follow-Up
Full credentialing and re-credentialing with all major payers, with managed timelines and status tracking so you never miss a network participation window.
A/R Reporting & Performance Tracking
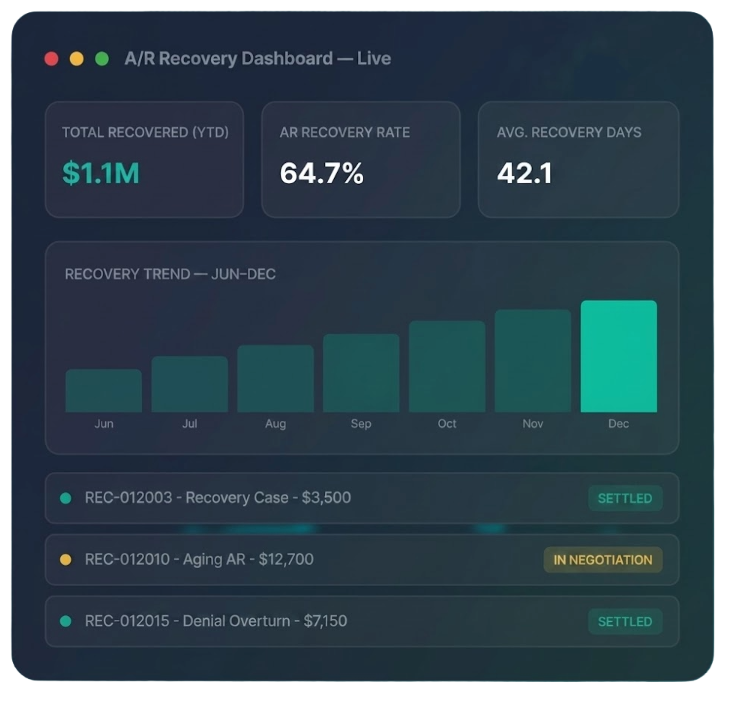
Real-time dashboards provide insights into aging trends, recovery rates, and payer performance — giving you complete control over your revenue.
Analytics & Reporting
Real-time KPI dashboards with payer mix analysis, denial trending, and collections benchmarking — full financial visibility for your leadership team.
— Key Benefits
Measurable Results That Define Our Standard
Clients experience quantifiable improvements in collections, claim resolution, and cash flow within the first 90 days of onboarding.
Maximized Revenue Recovery
Clients average 18% more collections than typical in-house billing — driven by comprehensive follow-up, denial management, and complete charge capture.
Lower Administrative Expenses
Save on salaries, training, software, and benefits. Horizon delivers expert A/R recovery at a fraction of in-house cost.
Faster Payment Turnaround
Same-day claim follow-up and strategic recovery processes ensure most clients see payments 40% faster after onboarding.
Complete Data Security & Compliance
Our HIPAA-trained staff, encrypted data handling, BAA agreements, and routine compliance audits safeguard your revenue and your patients’ data.
A Structured Path to Maximized Collections
Our proven 5-step methodology delivers measurable results from week one — with zero disruption to your existing workflow.
— Why Choose Horizon
The Strategic Advantage Over In-House Billing
In-house A/R teams are often costly, slow, and less effective at recovering outstanding revenue. Horizon Revenue Group delivers measurable results.
Specialty-Certified Recovery Experts
Our A/R specialists hold AAPC and AHIMA certifications across 10+ medical specialties — ensuring expert handling of denials, underpayments, and complex payer requirements.
Transparent, Real-Time A/R Reporting
24/7 access to your accounts receivable dashboards. No black box — track aging claims, recovery rates, and payer performance anytime.
Technology-Driven, Human-Executed
AI-powered claim analysis, denial prediction, and automated follow-ups — combined with expert A/R specialists managing every exception personally.
Dedicated Account Management
A named account manager familiar with your practice, payers, and recovery goals — always available by phone or email to ensure smooth collections and timely updates.

Horizon combines specialty-certified billing experts, AI-assisted denial prediction, and evidence-based escalation protocols. Unlike in-house teams, we focus exclusively on revenue recovery, delivering higher collection rates at lower operational cost.
All recovery activities follow HIPAA standards, payer-specific protocols, and internal audit checks. Denial appeals, claim corrections, and underpayment adjustments are documented and compliant, reducing exposure to audits or penalties.
Yes. By analyzing denied, underpaid, and delayed claims, Horizon identifies patterns in coding, documentation, and payer behavior — allowing you to fix root causes, prevent future losses, and optimize revenue cycle efficiency.
Our dashboards provide visibility into claim aging, recovery velocity, payer performance, and collection bottlenecks. CFOs can use these insights to adjust staffing, negotiate contracts, or forecast revenue — turning recovered dollars into strategic financial leverage.
— FAQs
Answers to Questions Your CFO Will Ask
Data-Driven Insights Your Finance Team Can Trust
— Start Today
Ready to Recover Every Dollar Your Practice Deserves?
Claim your free, no-obligation A/R recovery audit and see exactly how much revenue your practice can reclaim — with zero risk and immediate insights.
