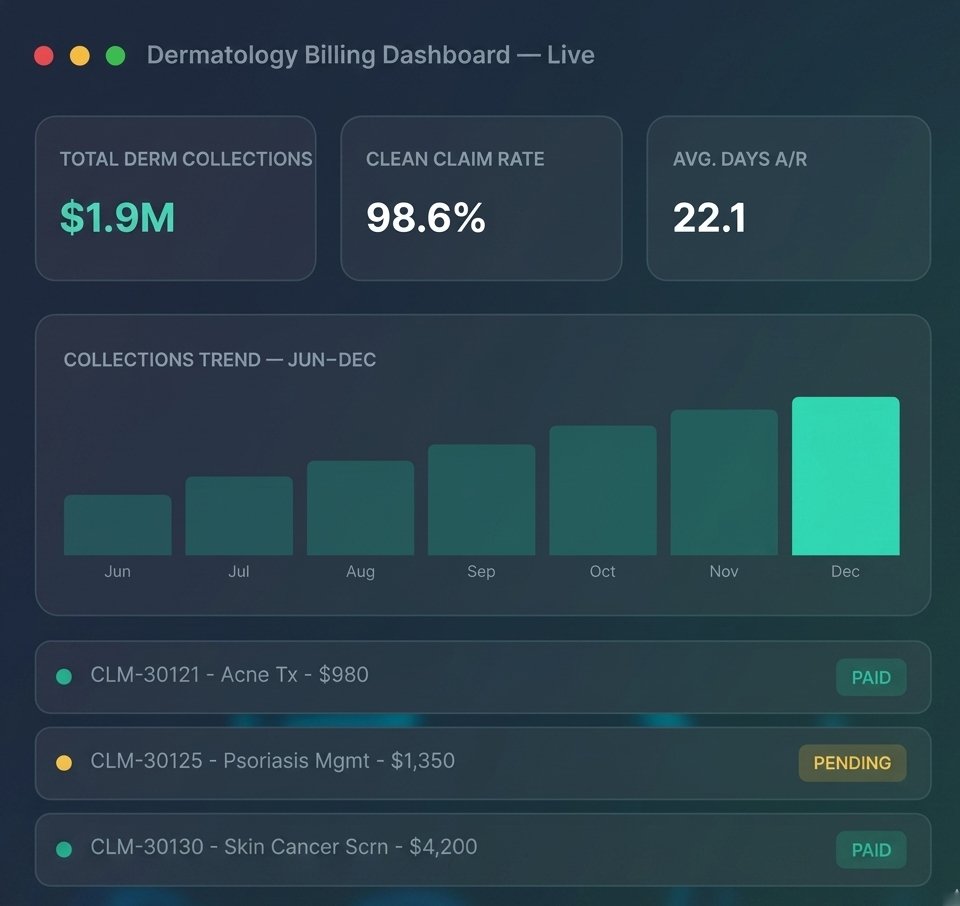
Dermatology Billing That Captures Every Clinical Dollar
HIPAA Compliant
Dermatology-Certified Coders
350+ Derm Practices Served
24-Hour Claim Submission
The Most Nuanced Coding in Outpatient Care — Mastered
Horizon Revenue Group's dermatology billing specialists bring deep expertise in CMS-1500 professional claim submission, CPT coding for integumentary procedures, HCPCS Level II coding for biologics and topical agents, and correct modifier application for bilateral and multiple lesion procedures. We don't apply generic billing templates — we build a revenue cycle engineered precisely for dermatology practice environments.
● CMS-1500 Submission
● Mohs & Excision Coding
● Biologics Billing
● Prior Auth Management
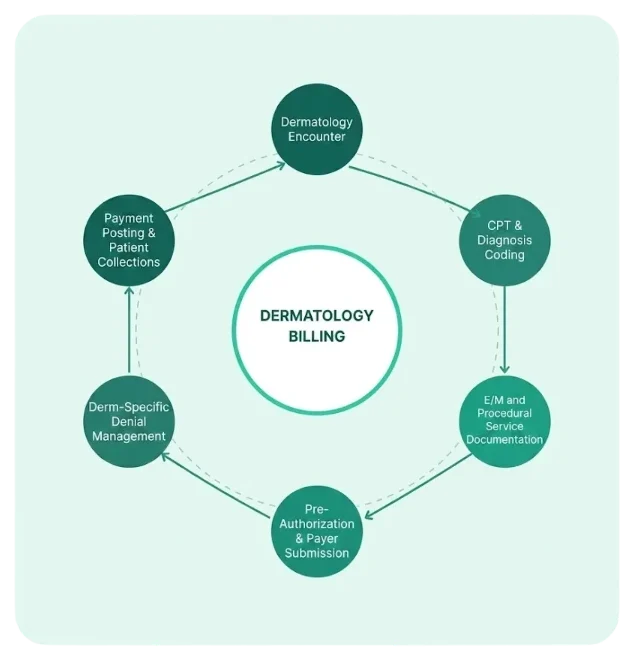
Why Dermatology Revenue Leaks Are Uniquely Costly
Medical vs. Cosmetic Misclassification
Incorrectly billing medically necessary procedures — such as actinic keratosis removal or benign lesion excision — as cosmetic results in immediate blanket denials, recovery audits, and potential compliance risk.
Mohs Surgery Multi-Stage Coding Errors
Mohs micrographic surgery requires precise stage-by-stage coding. Under-coding stages or misapplying reconstruction CPT codes leaves thousands uncollected per case, especially for complex melanoma and BCC procedures.
Biologic & Drug Billing Gaps
Biologics such as dupilumab, secukinumab, and ixekizumab require J-code billing, prior authorization, and step therapy documentation. Missing any element leads to full drug cost denials averaging $15,000+ per infusion.
Bundling & Multiple Lesion Modifier Errors
Improper use of -59, -XS, and -51 modifiers for multiple lesion procedures triggers automatic bundling edits, leaving significant revenue on the table for high-volume dermatology clinics performing 30+ procedures daily.

— Dermatology Services
Complete Dermatology Billing Coverage — Zero Gaps
Dermatology Prior Authorization
End-to-end prior authorization management for biologics, photodynamic therapy, laser treatments, and elective surgical procedures — including clinical documentation support, peer-to-peer coordination, and real-time status tracking.
Mohs & Surgical Procedure Coding
Certified dermatology coders accurately assign multi-stage Mohs CPT codes (17311–17315), reconstruction codes, and excision codes — ensuring every stage and closure is billed correctly and completely without triggering audit flags.
Biologic & Drug Infusion Billing
Complete J-code billing for dupilumab, secukinumab, ixekizumab, and all FDA-approved dermatologic biologics — with step therapy documentation, buy-and-bill coordination, and copay assistance program integration for maximum reimbursement.
CMS-1500 Claim Submission & Scrubbing
Professional claims scrubbed against dermatology-specific payer edits — including correct modifier application for bilateral lesions, multiple-procedure discounting rules, and anatomic site specificity — before same-day electronic submission.
Dermatology Denial Management & Appeals
Rapid denial triage within 48 hours with targeted appeals including pathology reports, pre-authorization records, operative notes, and clinical photographs — backed by payer-specific escalation protocols for dermatology procedures.
A/R Follow-Up & Aged Balance Recovery
Proactive follow-up on all outstanding dermatology claims, recovery of 60–180+ day aged balances, and coordination with pathology labs and ancillary service providers to resolve split-billing and coordination-of-benefits issues.
Dermatology Provider Credentialing
Full physician and mid-level provider credentialing with Medicare, Medicaid, and all major commercial payers — including CAQH maintenance, payer enrollment, and in-network contract analysis aligned to your procedure and payer mix.
Patient Estimates & Self-Pay Collections
Pre-visit patient cost estimations for dermatologic procedures, transparent itemized statements, automated payment reminders, and online payment portals — reducing self-pay bad debt and accelerating out-of-pocket collections.
Dermatology Analytics & Compliance Reporting
Real-time dashboards with procedure-level reimbursement benchmarking, cosmetic-versus-medical revenue split analysis, payer performance scorecards, and MIPS/Quality reporting support to protect your Medicare payment adjustments.
— Key Benefits
Measurable Outcomes for Dermatology Practices
Maximized Procedure-Level Reimbursement
Dermatology-credentialed coders ensure every lesion excision, Mohs stage, destruction procedure, and pathology service is correctly coded — recovering revenue that general medical billers consistently miss or underbill.
Eliminated Medical Necessity Denials
Proactive medical necessity documentation, ICD-10 linkage to procedure codes, and real-time eligibility verification prevent the costly denials that dermatology practices accept as routine when using non-specialist billers.
Full Biologic & High-Cost Drug Revenue Capture
Structured buy-and-bill and specialty pharmacy coordination workflows ensure that high-cost biologics for psoriasis, atopic dermatitis, and hidradenitis suppurativa are never left unbilled or reimbursed below cost.
Ongoing CMS & MIPS Compliance Support
Stay current with annual CPT code updates for integumentary procedures, CMS fee schedule changes, and MIPS quality measure reporting deadlines — with expert guidance embedded directly into your billing program.
A Structured Approach Built for High-Volume Derm Practices
— Why Choose Horizon for Dermatology Billing
Dermatology Expertise That General Billers Simply Don't Have
Dermatology-Credentialed Coding Specialists
Our coders hold AAPC Certified Professional Coder (CPC) credentials with dermatology-specific CEU training — with specialty expertise across Mohs surgery, surgical dermatology, cosmetic dermatology, and pediatric derm.
Payer-Specific Dermatology Contract Intelligence
We maintain current knowledge of payer-specific dermatology fee schedules, biologic carve-out arrangements, and prior authorization policy changes — ensuring you never leave contracted reimbursement uncollected.
Medical & Cosmetic Billing Differentiation
We precisely separate medically necessary from cosmetic services — maintaining compliant ICD-10 coding and documentation that maximizes reimbursable claims while protecting your practice from audit exposure.
MIPS & Quality Reporting Compliance Support
We track CMS MIPS quality measure updates, annual CPT integumentary code changes, and payer clinical policy revisions so your practice remains compliant and Medicare payment-optimized without administrative burden.
— FAQs
Dermatology Billing Questions — Answered
Clear, data-backed answers to the financial questions your CFO cares about most.
— Start Today
