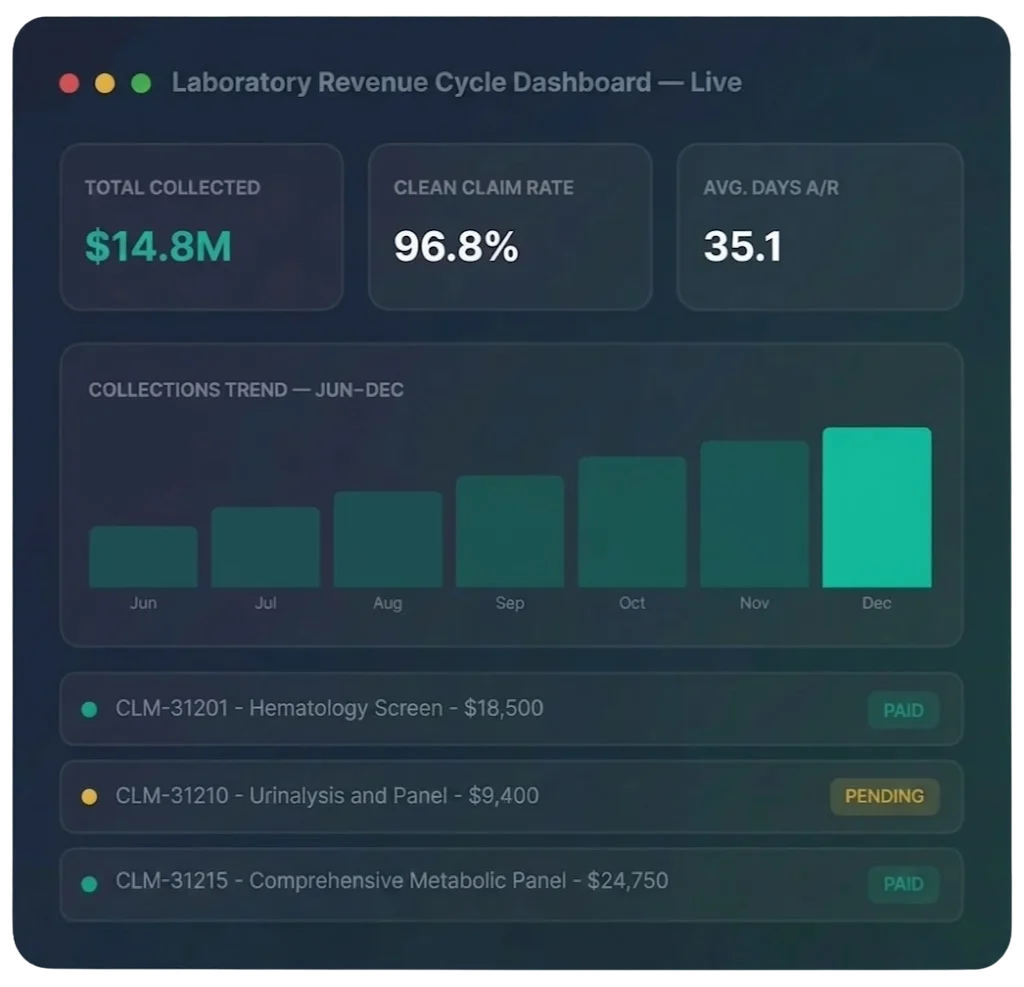
Lab Billing That Recovers Every Diagnostic Dollar
Clinical laboratories face uniquely complex billing challenges — PAMA-compliant pricing, LOINC coding, NPI-level specimen traceability, and payer-specific medical necessity requirements. Horizon Revenue Group specializes in lab billing to maximize collections and eliminate costly denials.
HIPAA Compliant
CLIA-Certified Coders
350+ Labs Served
24-Hour Claim Submission
The Most Regulation-Dense Billing in Healthcare — Mastered
Horizon Revenue Group's laboratory billing specialists bring deep expertise in CPT and HCPCS lab code assignment, Medicare CLFS fee schedule application, advance beneficiary notice workflows, and payer-specific LCD policy compliance. We don't apply general medical billing practices to your lab — we engineer a revenue cycle built specifically for diagnostic and clinical laboratory environments.
● PAMA Fee Schedule
● LCD Compliance
● Molecular & Genetic Coding
● ABN Management

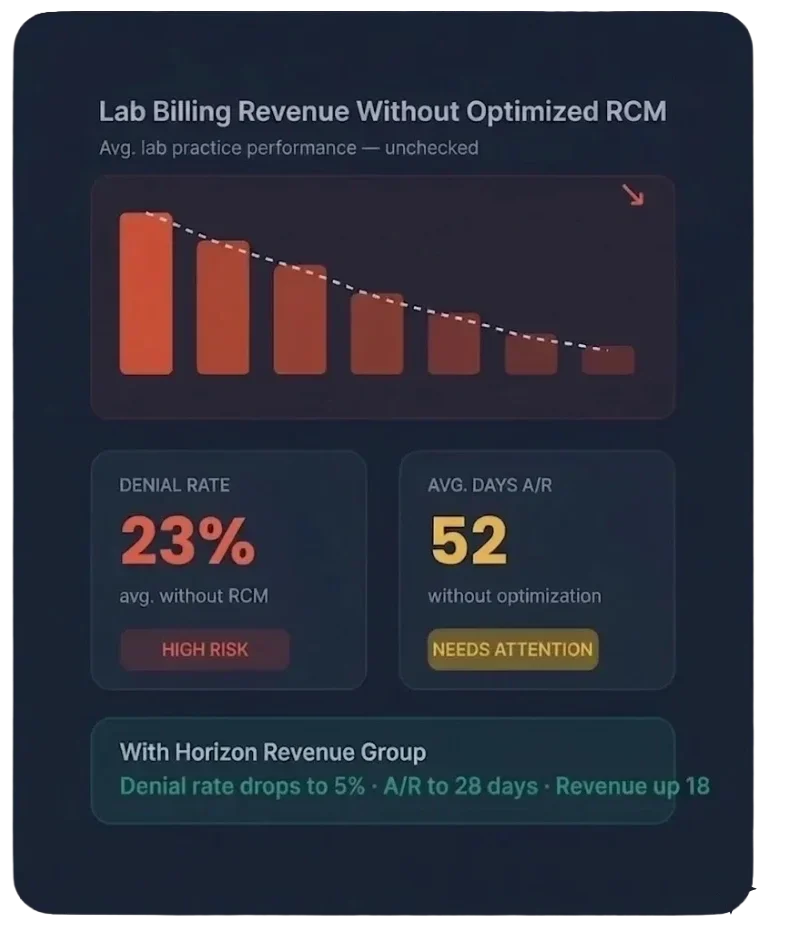
Why Lab Revenue Leaks Are Uniquely Costly
Laboratories operating without specialized billing expertise routinely lose 25–35% of collectable revenue to medical necessity denials, incorrect PAMA pricing, improper LCD compliance, and unbundled test coding.
Medical Necessity & LCD Non-Compliance
Tests ordered without supporting ICD-10 diagnosis codes that satisfy Local Coverage Determinations result in blanket Medicare denials — often representing the largest single source of preventable lab revenue loss.
PAMA Pricing & Fee Schedule Errors
Incorrectly applied PAMA-mandated Clinical Laboratory Fee Schedule rates — or failure to update rates with annual CMS revisions — silently erode lab reimbursement on every Medicare claim submitted.
CPT Unbundling & Reflexive Test Coding
Improperly bundled panel codes, missing reflex test modifiers, and incorrect molecular diagnostic tier assignments create audit exposure and leave substantial legitimate revenue on the table.
Missing ABN & Ordering Provider Gaps
Failure to issue timely Advance Beneficiary Notices for non-covered tests — combined with missing or invalid ordering provider NPIs — results in denied claims and unrecoverable patient liability for your laboratory.
Complete Lab Billing Coverage — Zero Gaps
Medical Necessity & LCD ReviewMedical Necessity & LCD Review
Pre-submission review of every test order against active Medicare Local Coverage Determinations and private payer policies — verifying that diagnosis codes fully satisfy medical necessity requirements before the claim is filed.
CPT & HCPCS Lab Code Assignment
Certified laboratory coders assign precise CPT Category I and HCPCS Level II codes — including molecular diagnostic tier mapping, panel bundling logic, and reflex test coding — to capture full allowable reimbursement on every test.
PAMA Fee Schedule Management
Precise application of CMS Clinical Laboratory Fee Schedule rates under PAMA regulations, updated annually with each rate revision cycle — ensuring your Medicare claims never underbill or expose the lab to PAMA audit risk.
Electronic Claim Submission & Scrubbing
Lab claims scrubbed against payer-specific edits — including NPI validation, ordering provider verification, specimen source codes, and diagnosis pointer rules — before same-day 837P electronic transmission to all payers.
Lab Denial Management & Appeals
Rapid denial analysis within 48 hours for all lab claim denials. Targeted appeals with requisition documentation, ordering provider attestations, and payer-specific LCD compliance evidence — with escalation protocols that recover revenue others write off.
ABN Management & Patient Billing
Systematic Advance Beneficiary Notice issuance workflows for all non-covered and frequency-limited tests, patient liability estimation, clear itemized lab statements, and online payment portals to accelerate out-of-pocket collections.
Lab Credentialing & Enrollment
Full laboratory credentialing and re-enrollment with Medicare, Medicaid, and all commercial payers — including CLIA certificate verification, PECOS enrollment, payer-specific lab agreements, and in-network contract negotiation.
A/R Follow-Up & Collections
Proactive follow-up on all outstanding lab claims, systematic recovery of aged balances 30–120+ days, and coordination with ordering providers to obtain missing documentation for stalled claims — minimizing write-offs.
Lab Analytics & Compliance Reporting
Real-time dashboards with test mix analysis, payer reimbursement benchmarking, PAMA rate impact reporting, ordering provider performance tracking, and CLIA compliance monitoring to keep your lab audit-ready at all times.
— Key Benefits
Measurable Outcomes for Clinical Laboratories
Maximized Test Reimbursement
Lab-specialized coders ensure every CPT code, molecular diagnostic tier, and reflex test is accurately mapped and billed — recovering the legitimate revenue that generic billers routinely fail to capture.
Eliminated Medical Necessity Denials
Proactive LCD review, ICD-10 diagnosis validation, and ABN issuance workflows prevent the medical necessity denials that most labs treat as unavoidable — turning them into collected revenue.
Full PAMA & Regulatory Compliance
Annual PAMA fee schedule updates, CLIA certification tracking, and ongoing payer policy monitoring built directly into your billing program — keeping your lab compliant without added administrative burden.
Reduced Audit Exposure
Proper molecular diagnostic tier assignment, correct panel bundling, and defensible documentation practices reduce your lab's exposure to OIG and payer audit activity — protecting long-term revenue integrity.
A Structured Workflow Built for High Test Volume
Lab Expertise That Generic Billing Companies Don't Have
CLIA-Credentialed Lab Coding Specialists
Our coders hold AAPC Certified Professional Coder (CPC) and laboratory-specific credentials — with deep expertise across molecular diagnostics, toxicology, anatomic pathology, and clinical chemistry.
Up-to-Date PAMA & LCD Policy Intelligence
We maintain a continuously updated library of Medicare LCD policies, PAMA fee schedule changes, and private payer lab coverage rules — so your claims are always coded and priced correctly from day one.
LIS & EHR System Integration
Seamless integration with your Laboratory Information System and EHR — enabling automated charge capture from resulted tests, eliminating manual data entry errors, and accelerating claim submission timelines.
Proactive OIG & Audit Risk Management
We monitor OIG Work Plans, CMS Transmittals, and payer prepayment audit trends affecting laboratories — adjusting your billing program proactively to minimize audit exposure and protect long-term Medicare certification.

Lab billing requires specialized CPT coding for diagnostic tests — including molecular diagnostic tier assignment, panel bundling rules, and reflex test modifiers — that differ entirely from surgical or E&M physician coding. It also demands PAMA fee schedule compliance, Local Coverage Determination adherence, CLIA certification verification, and ordering provider NPI validation on every claim. Applying the wrong billing logic to a laboratory results in chronic denials, audit exposure, and significant revenue loss.
— FAQs
Lab Billing Questions — Answered
Clear, data-backed answers to the financial questions your CFO cares about most.
— Start Today
Ready to Maximize Your Laboratory's Revenue?
Get a free, no-obligation lab revenue audit and discover exactly how much your clinical laboratory could be recovering.
