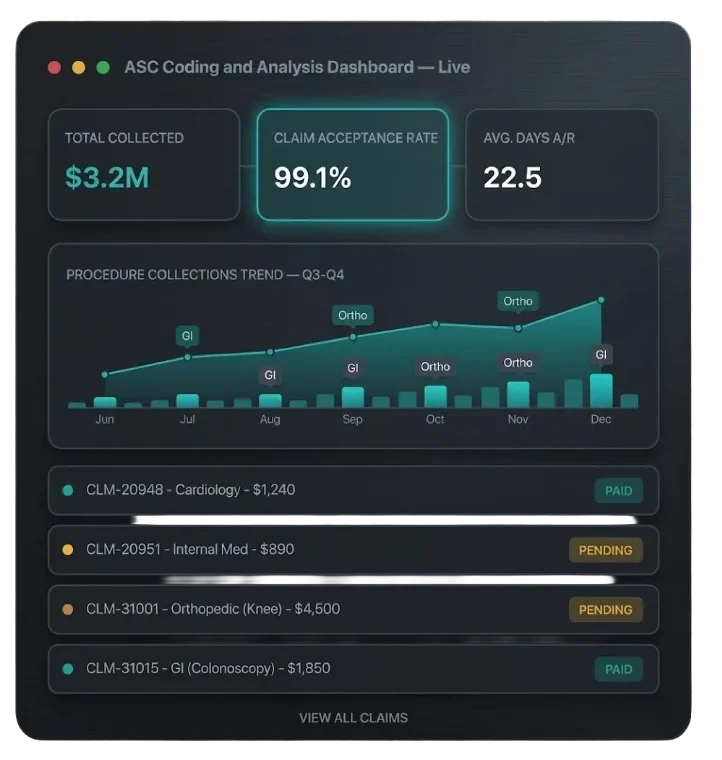
Medical Coding That Pays What You Actually Earned
HIPAA Compliant
CPC & CCS Certified Coders
30+ Specialties
48-Hour Chart Turnaround
The Clinical-to-Financial Bridge That Determines What You Get Paid
When coding is inaccurate, incomplete, or non-specific, the consequences are immediate: claim denials, payer audits, Medicare recovery demands, and chronic underpayment. Horizon Revenue Group provides AAPC and AHIMA-certified medical coders who specialize by clinical domain — not generic coders — to extract maximum legitimate reimbursement from every encounter while maintaining full compliance with CMS, AHA, and AMA coding guidelines.
● ICD-10-CM / PCS
● CPT & HCPCS Level II
● HCC Risk Adjustment
● E/M Optimization

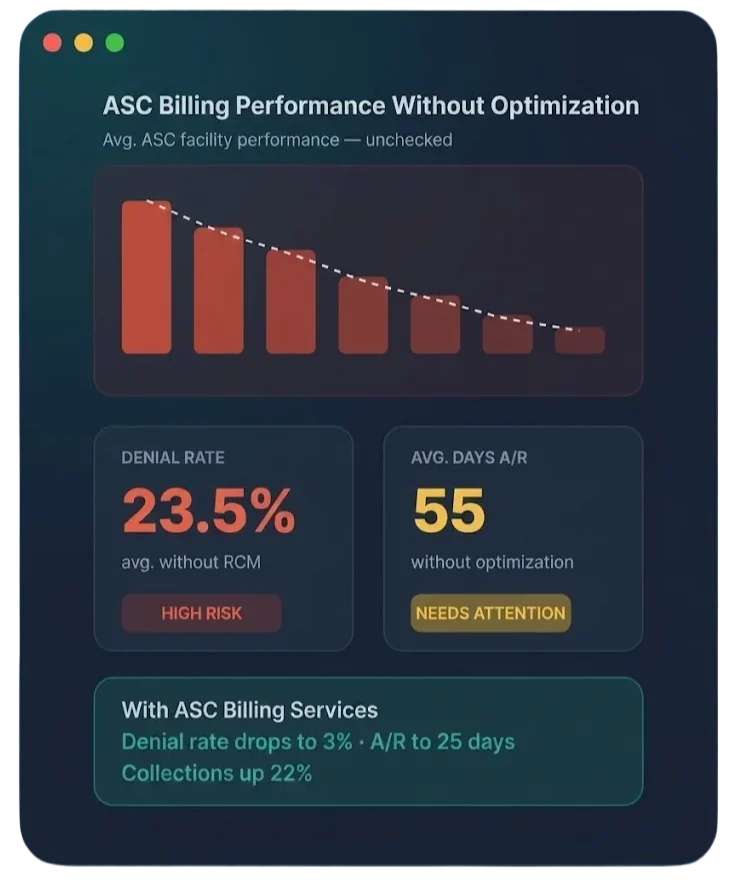
Why Coding Errors Are the #1 Cause of Healthcare Revenue Loss
Under-Coding & Non-Specific Diagnoses
Vague ICD-10 codes without required specificity result in systematic underpayment — payers reimburse at the lowest possible rate when documentation doesn't support a more specific code.
E/M Level Downcoding
Evaluation and management visits coded at lower complexity levels than documentation supports cost practices thousands per month in lost reimbursement — often without the provider ever knowing.
Missed HCC Capture & RAF Undercoding
For Medicare Advantage and value-based contracts, every uncaptured HCC condition reduces your risk-adjusted revenue and quality performance scores — permanently for that plan year.
Audit Exposure from Upcoding Risk
Inconsistent coding patterns trigger payer audits and RAC reviews. Without systematic coding quality controls, a single audit cycle can result in significant repayment demands and penalties.
Complete Medical Coding Coverage — Zero Gaps
ICD-10-CM / PCS Diagnosis Coding
Certified coders assign the highest-specificity ICD-10-CM diagnosis codes supported by clinical documentation — capturing acuity, comorbidities, and complication codes that directly impact reimbursement and quality scores.
CPT Procedure & E/M Coding
Precise CPT procedure code assignment with accurate modifier application — plus E/M level optimization using 2021 AMA guidelines to ensure office visit complexity is fully and compliantly captured for every encounter.
HCC Risk Adjustment Coding
Specialized HCC coding for Medicare Advantage and ACO value-based contracts — capturing all documented Hierarchical Condition Categories to optimize your Risk Adjustment Factor (RAF) score and ensure appropriate capitated revenue.
HCPCS Level II & Specialty Coding
Accurate HCPCS Level II code assignment for drugs, medical supplies, durable medical equipment, and specialty services — including J-codes for infusion therapy, Q-codes, and G-codes for quality reporting measures.
Coding Denial Review & Appeals
Rapid root-cause analysis of coding-related claim denials — with targeted appeals, corrected claims, and coder education feedback loops that eliminate recurring denial patterns and protect future reimbursement.
Prospective & Retrospective Chart Audits
Pre-billing prospective audits catch coding errors before claims are submitted. Retrospective audits identify systematic underpayment patterns and support corrected claim filings to recover historical revenue.
Clinical Documentation Improvement (CDI)
Embedded CDI specialists work directly with your physicians to close documentation gaps before coding occurs — improving query response rates, specificity, and the completeness of the medical record that drives every reimbursement decision.
Telehealth & Remote Visit Coding
Accurate coding for telehealth encounters using place-of-service codes, audio-visual modifiers (GT, 95), and payer-specific telehealth billing rules — keeping your virtual care revenue fully compliant and maximally reimbursed.
Coding Analytics & Compliance Reporting
Real-time dashboards tracking coder productivity, first-pass accuracy rates, denial root causes, E/M distribution patterns, and HCC capture rates — with monthly provider scorecards and CMS compliance benchmarking.
— Key Benefits
Measurable Outcomes From Certified Medical Coding
Maximum Reimbursement, Full Compliance
Our coders extract the highest-specificity, fully-documented codes for every encounter — increasing reimbursement without triggering audit exposure from upcoding or unsupported code assignment.
Reduced Audit Risk & RAC Exposure
Systematic QA processes, consistent coding patterns, and built-in compliance controls dramatically reduce your audit risk profile and shield your organization from costly Medicare Recovery Audit Contractor reviews.
Optimized HCC & Value-Based Performance
Comprehensive HCC capture across your Medicare Advantage population improves RAF scores, quality metrics, and shared savings performance — converting documentation gaps into recovered capitated revenue.
Scalable Coding Capacity Without Overhead
Scale your coding throughput with patient volume — without the cost, turnover, and training burden of in-house coding staff. Horizon provides surge capacity, specialty depth, and consistent quality at every volume level.
A Structured Workflow Built for Accuracy at Scale
Specialty Coding Depth That Generalist Vendors Can't Match
AAPC & AHIMA Dual-Credentialed Coders
Every Horizon coder holds active CPC, CCS, or specialty-specific credentials — with mandatory continuing education, annual re-certification, and specialty training aligned to your patient population.
Specialty-Matched Coder Assignment
We assign coders based on specialty expertise — your cardiology charts go to a cardiology coder, your oncology charts to an oncology coder. Specialty-specific nuance drives the accuracy difference that shows up on your bottom line.
Built-In CDI & Provider Education Loop
Our embedded CDI process doesn't just code what's there — it closes documentation gaps at the source, with provider-level education and query tracking that improves documentation quality over time.
Payer Intelligence & LCD/NCD Compliance
We maintain current knowledge of all major payer Local Coverage Determinations, National Coverage Determinations, and coding guidelines — so every code assigned is both clinically accurate and payer-compliant.

— FAQs
Medical Coding Questions — Answered
Clear, data-backed answers to the financial questions your CFO cares about most.
— Start Today
Ready to Stop Leaving Revenue on the Table?
Get a free, no-obligation medical coding audit and discover exactly how much your practice or health system could be recovering through more accurate, compliant coding.
