— Internal Medicine Billing & Revenue Cycle Management
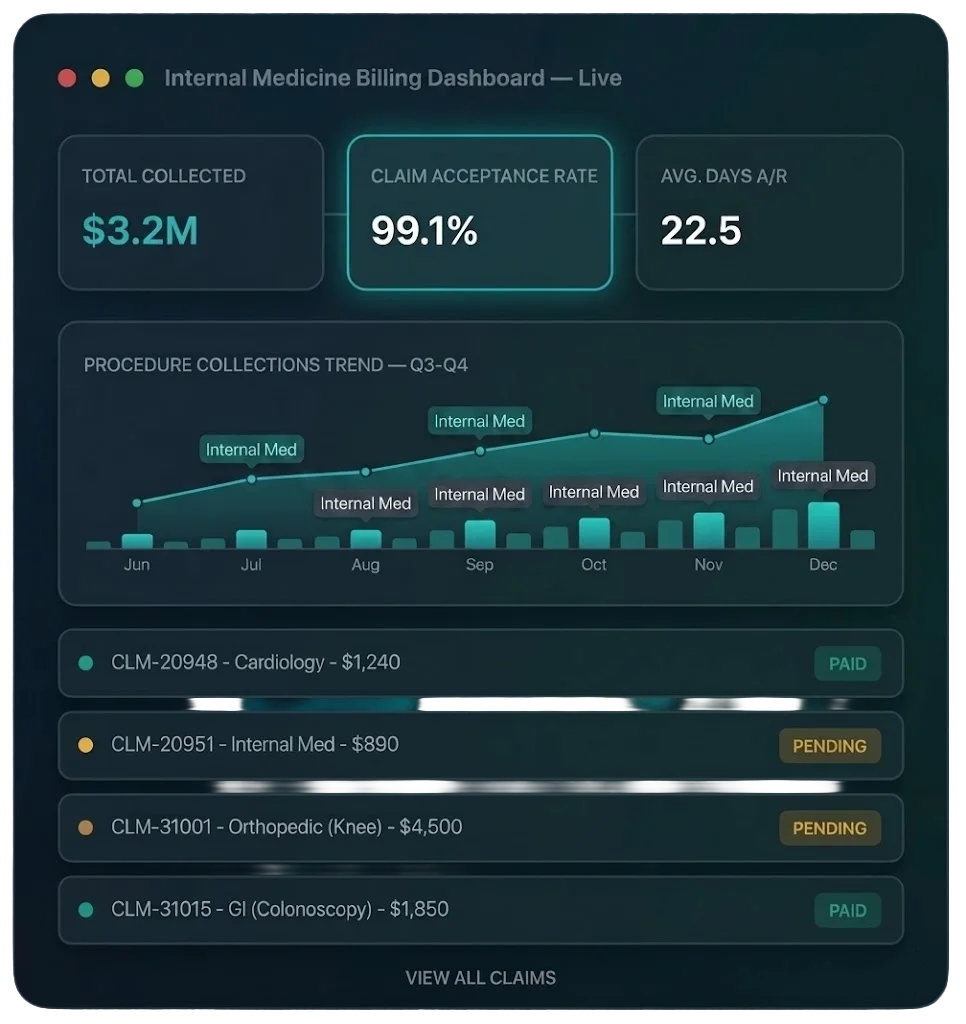
Internal Medicine Billing That Captures Every Patient Encounter
HIPAA Compliant
IM-Certified Coders
400+ IM Practices Served
Same-Day Claim Submission
The Broadest Coding Scope in Outpatient Medicine — Fully Managed
Horizon Revenue Group's internal medicine billing specialists bring proven expertise in 2021 AMA E&M guideline compliance, medical decision-making (MDM) level optimization, Medicare Advantage coding, preventive-versus-problem visit bundling rules, and CMS Quality Payment Program reporting. We don't guess at complexity levels — we engineer defensible, audit-ready claims that capture the full value of every physician encounter.
● E&M Level Optimization
● CCM & TCM Billing
● AWV & Preventive Coding
● MIPS / QPP Support

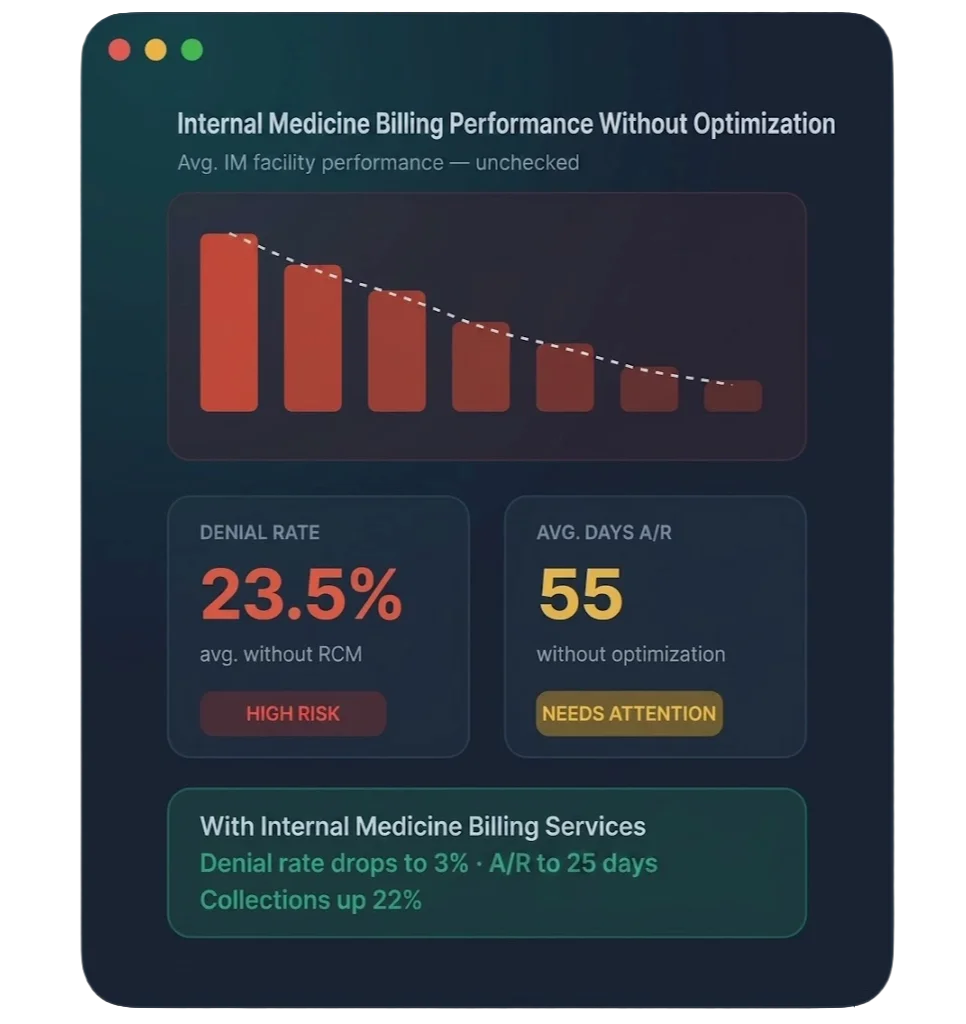
Why IM Practices Leave Significant Revenue Uncollected
Internal medicine practices relying on non-specialized billing support consistently undercode complex visits, miss billable care management services, and fail to capture preventive care revenue — losing an estimated 15–25% of collectible revenue every month.
E&M Undercoding & Complexity Misassignment
The 2021 AMA E&M guideline changes shifted coding to medical decision-making and total time — creating widespread undercoding in practices still using outdated documentation habits, leaving significant reimbursement per visit uncaptured.
Missed Chronic Care & Transitional Care Revenue
CCM (99490), TCM (99495/99496), and RPM (99457) codes represent thousands in monthly recurring revenue that most internal medicine practices either never bill or routinely lose to documentation and enrollment failures.
Preventive Visit Bundling & Modifier Errors
Incorrectly bundling Annual Wellness Visits with problem-oriented E&M services — or failing to apply modifier -25 when both are rendered on the same date — results in systematic denial of one service or the other across your entire patient panel.
MIPS / QPP Non-Compliance Penalties
Internal medicine physicians participating in Medicare's Quality Payment Program face payment adjustments of up to 9% for incomplete MIPS reporting. Without active QPP management, these penalties compound annually — directly reducing your Medicare revenue.
Complete IM Billing Coverage — Zero Gaps
E&M Coding & Level Optimization
Expert application of 2021 AMA E&M guidelines using medical decision-making (MDM) and total physician time — ensuring every office visit, hospital encounter, and consultation is coded at the highest defensible level with complete audit-ready documentation alignment.
Chronic Care Management (CCM) Billing
End-to-end CCM program billing for patients with two or more chronic conditions — including 99490, 99491, 99487, and 99489 billing, patient enrollment documentation, care plan requirements, and monthly time log verification to capture this high-value, recurring revenue stream reliably.
Annual Wellness Visit & Preventive Coding
Accurate coding of Medicare Annual Wellness Visits (G0438, G0439), Initial Preventive Physical Exams (G0402), and same-day problem visit add-ons with correct modifier -25 application — preventing the bundling denials that silently eliminate preventive care reimbursement across your patient panel.
Transitional Care Management (TCM) Billing
Full TCM billing workflow for patients discharged from hospital, SNF, or observation — including 99495 and 99496 documentation requirements, mandatory contact timeframes, face-to-face visit tracking, and coordination with inpatient billing to eliminate conflicting claim submissions.
Denial Management & Appeals
Rapid review of all internal medicine claim denials — including E&M complexity downcoding appeals, preventive visit bundling disputes, medical necessity denials with clinical documentation support, and Medicare Advantage plan-specific escalation protocols to recover every legitimately earned dollar.
Remote Patient Monitoring (RPM) Billing
Complete RPM program billing using 99453, 99454, 99457, and 99458 — including device setup documentation, monthly data review time verification, and patient engagement tracking — converting your RPM clinical program into a reliable, high-margin recurring revenue source.
Physician Credentialing & Enrollment
Full credentialing and re-credentialing for internists with Medicare, Medicaid, and all commercial payers — including CAQH profile management, Medicare Advantage enrollment, hospital privileges coordination, and group NPI enrollment to eliminate coverage gaps that delay reimbursement.
MIPS / QPP Reporting & Compliance
Active management of your Medicare Quality Payment Program participation — including MIPS measure selection, data submission, Promoting Interoperability reporting, Improvement Activities tracking, and performance score optimization to avoid payment penalties and pursue bonus incentives.
Practice Analytics & Revenue Reporting
Real-time dashboards with E&M level distribution analysis, payer mix performance benchmarking, CCM and RPM enrollment and revenue tracking, provider productivity reporting, and payer contract reimbursement analysis — giving your practice leadership complete financial visibility and actionable insights.
— Key Benefits
Measurable Outcomes for Internal Medicine Practices
Higher Reimbursement Per Encounter
E&M-specialized coders review every note against 2021 MDM criteria and total physician time documentation — consistently identifying and correcting undercoded visits to recover the full reimbursement each encounter clinically supports.
Unlocked CCM & RPM Revenue Streams
Most internal medicine practices have the patient population to generate significant monthly CCM and RPM revenue but lack the billing infrastructure to capture it. Horizon builds and manages the complete billing workflow to convert these programs into reliable monthly cash flow.
Zero Preventive Care Revenue Left Behind
Precise AWV, IPPE, and problem-visit add-on coding with correct modifier application ensures your preventive care services are always billed and always reimbursed — eliminating the bundling denials that cost IM practices thousands in Medicare preventive revenue each year.
Full MIPS Protection & Incentive Capture
Active QPP management protects your Medicare revenue from negative payment adjustments while positioning your practice to earn positive MIPS incentive payments — turning a compliance burden into a financial opportunity.
A Structured Workflow Built for High-Volume Physician Practices
IM Billing Precision That General Medical Billers Can't Deliver
2021 E&M Guidelines Experts
Our coders are fully trained on AMA's revised E&M guidelines — using MDM documentation and total physician time to code every visit at its highest appropriate level, consistently outperforming template-based coding approaches.
HCC & Medicare Advantage Coding Expertise
We capture all relevant Hierarchical Condition Category (HCC) diagnoses for Medicare Advantage patients — ensuring complete risk adjustment documentation that protects your practice's capitation revenue and accurately reflects patient complexity.
Dedicated CCM & RPM Revenue Program Management
Beyond billing, we help you identify eligible patients, build enrollment workflows, and track monthly qualifying time — transforming CCM and RPM from underutilized programs into consistent five-figure monthly revenue generators for your practice.
Proactive MIPS Score Optimization
Our QPP team selects the highest-scoring MIPS measures for your patient population, monitors your performance throughout the performance year, and submits data before CMS deadlines — eliminating negative adjustments and targeting incentive payments.

— FAQs
Internal Medicine Billing Questions — Answered
Clear, data-backed answers to the financial questions your CFO cares about most.
— Start Today
Ready to Maximize Your Internal Medicine Practice Revenue?
Get a free, no-obligation revenue audit and discover exactly how much your practice is leaving on the table — from undercoded E&M visits to uncaptured CCM and RPM billing.
