— Insurance Eligibility
Verify Coverage Before Every Visit
HIPAA Compliant
Certified Billers
Full Cycle Coverage
500+ Practices Served
— What Is Insurance Verification?
The First Line of Defense for Your Revenue Cycle
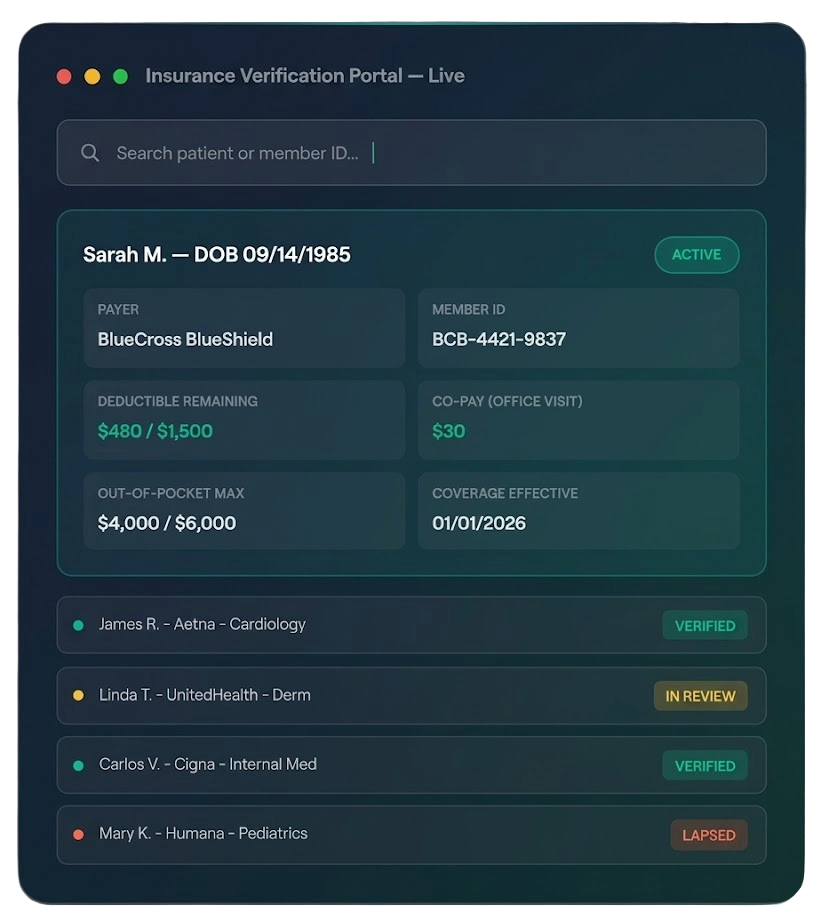
When verification is skipped or done manually, practices face costly claim denials, underpaid services, and frustrated patients who weren't informed of their financial responsibility. Horizon's dedicated verification team contacts payers directly and through electronic channels to collect the exact coverage data your billing team needs — before the encounter, every time.
● Real-time eligibility checks
● Benefits breakdown
● Prior auth flagging
● Patient responsibility
— The Problem
What Skipped Verification Is Costing Your Practice
Studies show that up to 75% of claim denials are caused by eligibility and registration errors — most of which are entirely preventable at the front end.
Eligibility-Related Claim Denials
Submitting claims without confirming active coverage is the leading cause of front-end denials, leading to costly rework cycles and delayed payments.
Patient Billing Disputes & Bad Debt
Patients who weren't informed of their financial responsibility before service are more likely to dispute balances, delay payment, or default entirely.
Coding Errors & Under-Billing
Procedures performed without required pre-authorization result in full claim rejections that are often not recoverable — lost revenue with no recourse.
Staff Overloaded with Manual Calls
Front desk staff spending hours each day on hold with payers is not scalable — it diverts resources from patient care and introduces manual verification errors.

— What's Included
Everything Your Practice Needs to Verify Right
A complete insurance verification suite — covering every payer, every plan, every patient, before every visit.
Real-Time Eligibility Verification
Automated, real-time eligibility checks against 900+ payers via EDI 270/271 transactions — confirming active coverage for every scheduled patient within hours of scheduling.
Benefits Detail Extraction
We retrieve the complete benefits picture: deductibles, co-pays, co-insurance percentages, out-of-pocket maximums, plan limitations, and specialty benefit tiers — formatted for your billing team.
Prior Authorization Management
We identify services requiring pre-authorization and initiate the auth request on your behalf — tracking status, managing peer-to-peer calls, and alerting your team before the procedure date.
Patient Responsibility Calculation
Accurate, upfront patient cost estimates based on verified benefits and procedure codes — enabling your front desk to collect the right co-pay at time of service, every time.
Secondary & Tertiary Coverage Check
We verify all active coverage layers — primary, secondary, and tertiary insurances — and confirm coordination of benefits (COB) rules to maximize total reimbursement on each claim.
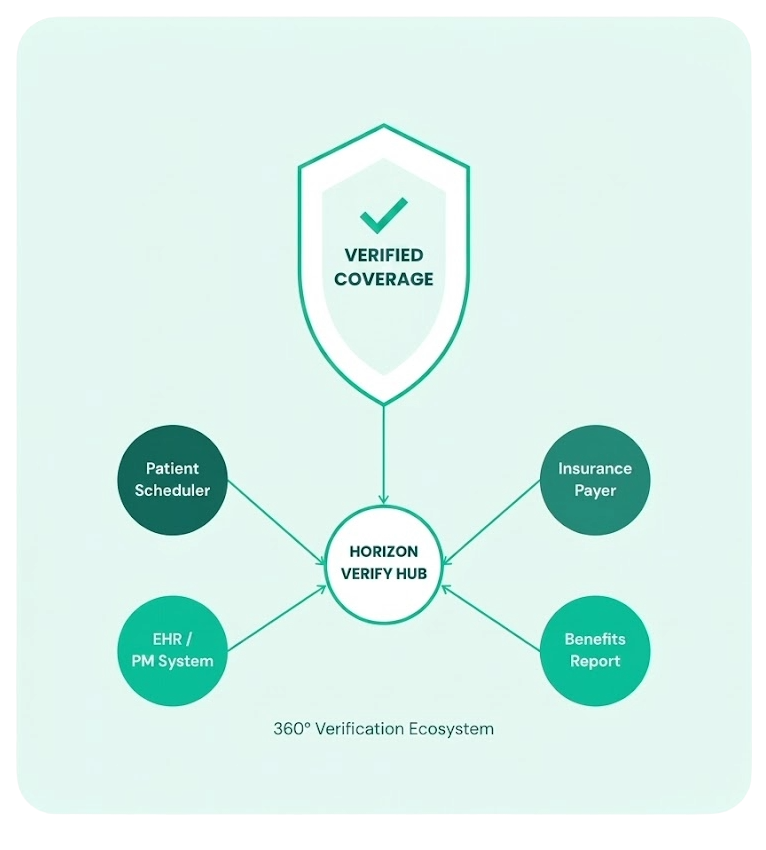
EHR-Integrated Reporting
Verification results are pushed directly into your EHR or practice management system in structured formats — no manual data entry, no information gaps, no workflow disruption.
— Key Benefits
Why Verification-First Practices Collect More
Front-end accuracy is the highest-ROI investment in your revenue cycle. Practices that verify every patient before every visit consistently outperform those that don't — across every financial metric.
Eliminate Eligibility-Based Denials
The single largest driver of claim denials — coverage gaps, terminated plans, and inactive member IDs — is completely eliminated when every patient is verified before the visit.
Improve Patient Financial Experience
When patients are informed of their exact co-pay and deductible obligation before their appointment, satisfaction improves, disputes decrease, and collections at time of service increase significantly.
Free Up Front-Desk Staff
Eliminate hours of manual verification calls. Our team handles every check so your staff can focus entirely on patient experience, scheduling, and clinical coordination.
Accelerate Clean Claim Submission
Verified eligibility data flows directly into the billing workflow, reducing errors at the coding and submission stage and supporting a 98%+ clean claim rate from day one.
— Our Verification Process
Five Steps to Verified, Denial-Proof Encounters
Our structured insurance verification workflow is triggered at scheduling and completed before every encounter — with zero manual effort from your team.
— Why Horizon
Built for Scale, Precision, and Practice Growth
Horizon's insurance verification service is not a bolt-on feature — it's a fully managed, dedicated function staffed.
900+ Payer Relationships
We maintain active relationships and EDI connections with virtually every commercial, Medicare, Medicaid, and managed care payer — no payer is too obscure.
Specialty-Trained Verification Staff
Our team is trained on specialty-specific benefit nuances, carve-out plan , and payer-specific pre-auth triggers.
Seamless EHR Integration
Seamless EHR Integration Verified data is delivered directly into your PM or EHR system — eliminating duplicate data entry and ensuring your billing team
Real-Time Escalation Protocol
When issues arise — inactive plans, missing auth, COB conflicts — our team escalates immediately with a resolution path, not just an alert, so your workflow never stalls.

Yes. Our team identifies services that require prior authorization based on the patient's plan and the procedure being performed. We initiate the auth request, track its status, manage peer-to-peer reviews when needed, and notify your team of approval or denial with next steps — before the appointment date.
Our team immediately escalates the issue with a clear action plan: we contact the patient with updated insurance information requests, notify your front desk with a coverage summary and recommended self-pay or alternative options, and document the finding so the billing team can adjust the encounter before claim submission — stopping denials before they happen.
— FAQs
Insurance Verification Questions, Answered
Clear, data-backed answers to the financial questions your CFO cares about most.
— Get Started Today
Stop Losing Revenue to Preventable Denials
Let Horizon verify every patient before every visit. Get a free eligibility audit and see exactly how much your practice could recover.
