— End-to-End Denial Management Services
Recover Every Dollar You’ve Earned
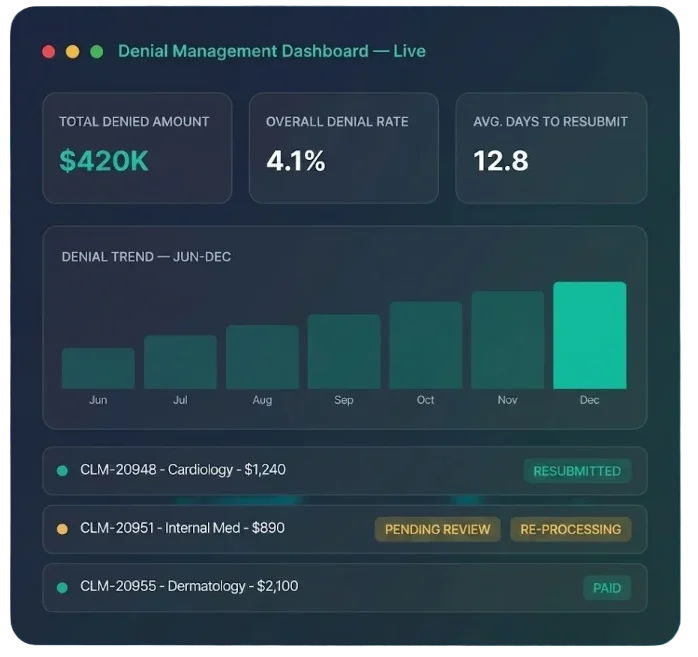
Horizon Revenue Group specializes in denial prevention and recovery, handling every step from claim submission review to appeals and payment posting — reducing denials, accelerating reimbursements, and delivering full financial visibility.
HIPAA Compliant
Certified Billers
Full Cycle Coverage
500+ Practices Served
— What We Do
Complete Denial Management for Your Practice
Denial management is the backbone of financial stability. Horizon handles every aspect — identifying potential denials, filing appeals, and preventing future claim rejections — so your team focuses on patients, not paperwork.
Our specialists bring deep experience across cardiology, internal medicine, dermatology, mental health, pediatrics, and more. We don’t just manage denials — we engineer a system that ensures every valid reimbursement is captured, consistently.
● Full-Service Denial Oversight
● HIPAA Compliant
● 24-Hour Appeal Response
● Live Performance Dashboards

— Core Services
End-to-End Denial Recovery, Designed to Maximize Revenue
High Denial Rates Impact Collections
Incorrect coding, incomplete documentation, and payer errors directly reduce revenue and overload staff with repetitive tasks.
Slow Payment Recovery
Extended denial cycles restrict cash flow, hinder operations, and slow your practice’s growth potential.
Missed Recovery Opportunities
Unmanaged denials quietly reduce monthly collections — often thousands of dollars without any visibility into lost revenue.
Strained In-House Teams
Staff spending hours on appeals and follow-up have less time for patient care and clinical coordination.
— Services Included
Every Step of Denial Management Covered
A full-service denial recovery program — nothing left unaddressed, no claims overlooked.
Pre-Submission Claim Review
We screen every claim to detect coding errors, documentation gaps, and payer-specific requirements, reducing preventable denials before submission.
Certified Coding Accuracy (ICD-10 / CPT)
Our coders flag potential denial risks and ensure claims are optimized for approval.
Claim Scrubbing & Submission
Claims are scrubbed against thousands of payer edits and electronically submitted within 24 hours, minimizing rejections.
Denial Resolution & Appeals
All denied claims are addressed within 48 hours using strategic appeals. Root causes are tracked to prevent repeat denials and improve clean claim rates.
A/R Follow-Up & Payment Recovery
Active follow-up on aged claims with escalation protocols ensures faster recovery and reduces days in accounts receivable.
Provider Credentialing
Complete credentialing and re-credentialing with major payers to prevent network-related denials.
Patient Statements & Billing
Clear, compliant statements with online payment portals and reminders, protecting revenue while maintaining patient trust.
Underpayment Identification & Recovery
We analyze payer reimbursements against contracted rates to identify underpayments and missed revenue.
Analytics & Reporting
Real-time dashboards tracking denial trends, appeal success rates, and recovered revenue for full financial transparency.
— Key Benefits
Proven Results That Deliver Impact
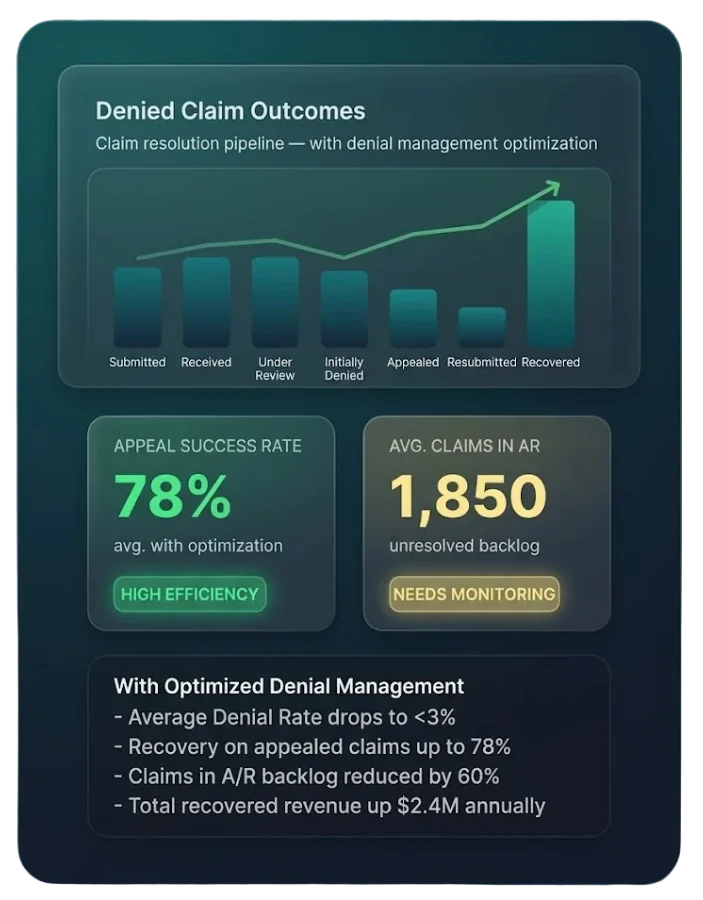
Clients experience noticeable improvements in denial rates, successful appeals, and revenue recovery within the first 90 days.
Stronger Revenue Recovery Performance
Practices achieve significantly higher recovered revenue compared to in-house teams — driven by proactive denial prevention, strategic appeals, and precise claim optimization.
Reduced Administrative Burden
Eliminate the overhead of maintaining an internal billing team. From staffing and training to software costs, we streamline operations while delivering expert-level denial management.
Enterprise-Grade Data Security & Compliance
Our processes are built around strict HIPAA standards, including secure data handling, encrypted systems, BAA agreements, and routine compliance monitoring.
Improved Cash Flow Velocity
Faster claim resolution, consistent follow-ups, and timely appeals help convert outstanding balances into payments much quicker than traditional workflows.
— Our Process
A Clear, Proven Approach to Denial Recovery
Our structured 5-step methodology delivers measurable results from day one — with zero disruption to your workflow.
— Why Choose Horizon
The Advantage Over In-House Teams
Internal denial management is often costly, inefficient, and inconsistent.
Certified Denial Specialists
AAPC and AHIMA-certified experts across 10+ specialties — focused on preventing and recovering denials.
Transparent, Real-Time Reporting
24/7 dashboard access with live tracking of denial trends, appeal outcomes, and recovered revenue.
Tech-Enabled, Human-Driven
AI-assisted denial prediction and claim scrubbing, executed personally by experienced staff.
Dedicated Account Management
A named manager familiar with your practice, payers, and revenue goals — available anytime.

All denied claims are reviewed and actioned within 24–48 hours. Our team prioritizes high-value and time-sensitive denials, ensuring faster appeal submissions and minimizing delays in reimbursement.
Our approach is both preventive and corrective. We identify risk factors before claims are submitted while also aggressively managing and appealing existing denials — creating a complete denial lifecycle solution.
Our denial specialists use payer-specific appeal strategies, detailed documentation, and data-backed justification for every claim. Combined with continuous tracking of payer behavior, this allows us to significantly improve appeal approval rates.
Yes. You’ll have access to real-time dashboards that provide full transparency into denial rates, root causes, appeal outcomes, and recovered revenue — enabling better financial decision-making for your practice.
— FAQs
Answers to Questions Your CFO Will Ask
Clear, data-backed answers to the financial questions your CFO cares about most.
— Start Today
Ready to Recover Lost Revenue from Denials?
Request a free, no-obligation denial audit and uncover exactly how much revenue your practice can recover from unpaid and underpaid claims.
