Precision Billing for Rheumatology Practices That Can't Afford Denials
HIPAA Compliant
CPC-Certified Coders
140+ Rheumatology Practices
24-Hour Submission
Specialized Revenue Cycle Management for Rheumatology's Unique Challenges
Our AAPC-certified rheumatology coders bring deep expertise across inflammatory arthritis, autoimmune disease management, infusion therapy, and musculoskeletal procedures. We don't just submit claims — we build a systematic revenue engine that captures every infusion minute, every drug unit, and every ancillary service your practice delivers.
● Infusion Therapy Billing
●Biologic Drug Administration
● Joint Injection Coding
● Chronic Disease Management

Why Rheumatology Practices Hemorrhage Revenue Every Month
Biologic Prior Authorization Failures
Payers require step therapy documentation and clinical justification for every biologic. Missing or incomplete PA submissions result in automatic denials on claims worth $5,000–$25,000 per infusion session.
Infusion Time & Drug Waste Errors
Infusion billing requires precise time-based coding (first hour vs. additional hours) and proper drug waste documentation. Miscoded infusion intervals silently erase tens of thousands in monthly revenue.
J-Code Complexity & Drug Dosing Errors
Incorrect J-code selection, wrong unit billing, and missed drug waste claims result in systematic underpayment on every biologic encounter — often undetected until a full revenue audit reveals months of losses.
Chronic Disease E&M Under-Coding
Rheumatologists managing complex multi-system autoimmune conditions routinely under-code E&M visits — missing the documentation threshold for higher-level codes that can add $80–$120 per encounter.

Complete RCM for Every Rheumatology Encounter
Infusion Therapy Billing
Precise time-based infusion coding for initial hours (96413) and additional hours (96415), including sequential infusion, concurrent infusion, and push administration — with complete drug waste documentation for every biologic encounter.
Biologic & J-Code Billing
Expert J-code selection and unit calculation for all major rheumatology biologics — infliximab (J1745), tocilizumab (J3262), abatacept (J0129), rituximab (J9312), and all other infused and injectable DMARDs with correct per-unit billing.
Prior Authorization Management
End-to-end PA management for all biologic therapies — initial submissions, step therapy documentation, peer-to-peer reviews, and urgent appeals. We track every PA status in real time and alert your team before any authorization expires.
Rheumatology Denial Management
Aggressive appeal strategy for rheumatology-specific denial reasons — step therapy non-compliance, medical necessity, infusion coding disputes, and drug coverage exclusions — with a 93%+ overturn rate and systematic root cause tracking.
Joint Injection & Procedure Coding
Accurate CPT coding for arthrocentesis and joint injections (20600–20611), trigger point injections, soft tissue injections, and ultrasound-guided procedures with correct Modifier 26 and imaging guidance add-on codes.
Chronic Disease E&M Coding
Optimized E&M coding (99202–99215) for rheumatoid arthritis, lupus, psoriatic arthritis, and other complex autoimmune conditions — ensuring medical decision-making complexity is fully documented and correctly leveled for maximum reimbursement.
Rheumatology Credentialing
Complete provider credentialing and re-credentialing with Medicare, Medicaid, and all major commercial payers — with specialty-specific rheumatology network enrollment and specialty drug program participation management.
Diagnostic Lab & Imaging Billing
Accurate billing for rheumatology diagnostic panels — ANA, anti-dsDNA, RF, anti-CCP, complement levels, HLA-B27, and musculoskeletal ultrasound — with correct Modifier 26/TC application and LCD compliance.
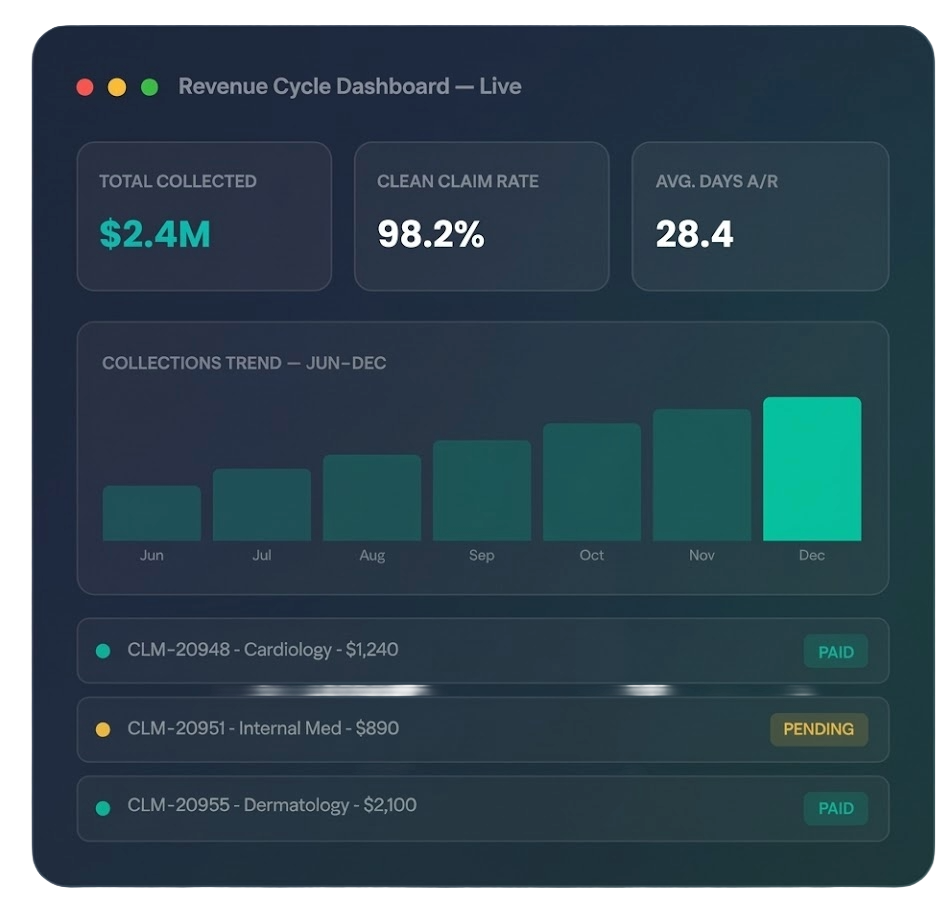
Rheumatology Analytics & Reporting
Real-time dashboards segmented by drug/procedure, payer, and provider — with infusion suite profitability analysis, biologic denial trending, and A/R benchmarking against rheumatology specialty peers.
— Key Benefits
Why Rheumatology Practices Choose Horizon
Maximum Infusion Revenue Capture
Our infusion billing specialists capture every billable hour, every drug unit, and every drug waste allowance — recovering an average of $15,000–$22,000 per physician monthly that generalist billers routinely miss in rheumatology infusion suites.
Proactive Prior Authorization Compliance
We manage every biologic PA proactively — including step therapy documentation, clinical criteria matching, and renewal tracking — ensuring no infusion is ever delayed or denied due to an authorization gap.
Payer-Specific Biologic Coverage Intelligence
We maintain payer-specific biologic coverage policies, formulary requirements, and step therapy criteria for every major insurer — applied pre-submission to prevent denials before they happen.
Infusion Suite Profitability Optimization
Our analytics team benchmarks your infusion suite revenue against rheumatology peers and identifies scheduling, coding, and payer mix opportunities to maximize the profitability of your in-office drug administration program.
A Purpose-Built Process for Rheumatology Revenue
The Rheumatology Billing Partner Built for Biologic-Driven Practices
Certified Rheumatology Infusion Coders
Our coders hold CPC credentials with dedicated rheumatology and infusion therapy experience — understanding J-code billing, drug waste rules, and time-based infusion coding at the clinical level.
Biologic Coverage Intelligence Library
We maintain continuously updated payer-specific biologic coverage policies, formulary tiers, step therapy requirements, and PA criteria — applied proactively to every claim before submission.
Zero Infusion Revenue Left Behind
Our systematic infusion charge capture review identifies every missed drug waste allowance, under-documented infusion hour, and uncaptured concurrent infusion — turning lost revenue into real collections.
Infusion Suite–Focused Account Management
Your named account manager specializes in rheumatology and infusion therapy billing — understanding your biologic mix, your payer contracts, and the unique revenue dynamics of your infusion program.
— FAQs
Rheumatology Billing Questions — Answered
Clear, data-backed answers to the financial questions your CFO cares about most.
— Start Today
