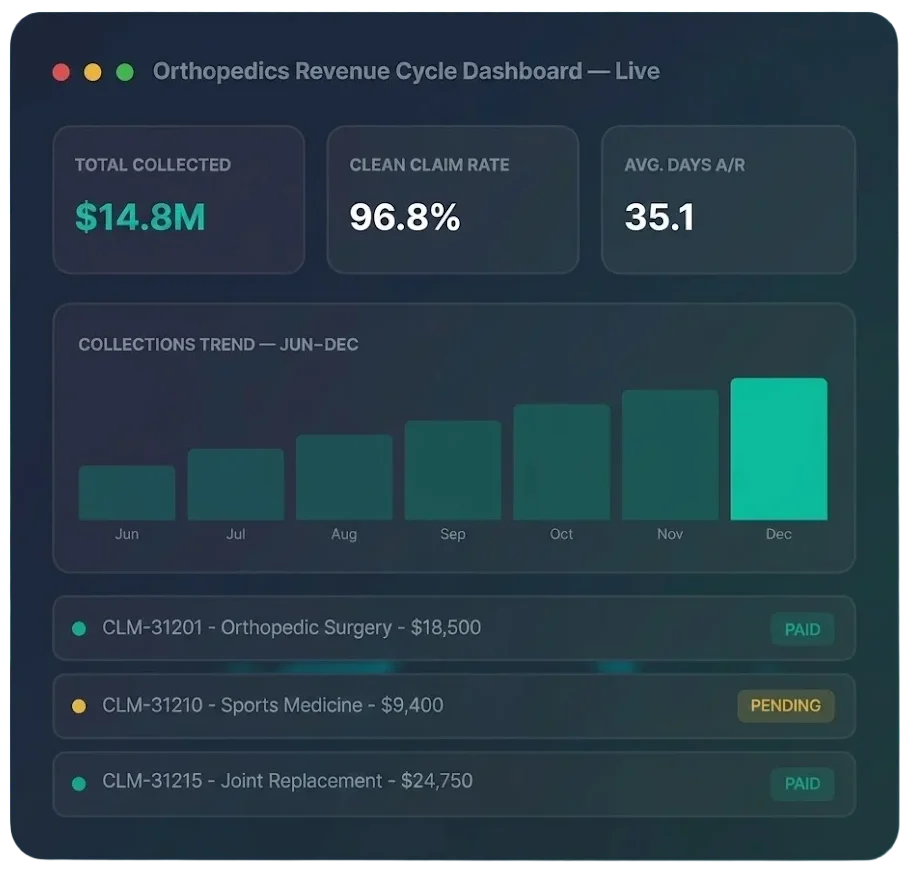
Orthopedic Billing That Recovers Every Procedure Dollar
HIPAA Compliant
COC-Certified Coders
350+ Ortho Providers
48-Hour Claim Submission
The Most CPT-Intensive Specialty in Medicine — Expertly Managed
Horizon Revenue Group's orthopedic-specialized billing team brings deep expertise in musculoskeletal CPT coding, CMS fee schedule optimization, global period management, Workers' Compensation billing protocols, and no-fault insurance adjudication. We engineer a revenue cycle purpose-built for high-volume orthopedic surgical and office-based environments.
● Musculoskeletal CPT Coding
● Global Period Management
● Implant & Hardware Billing
● Workers' Comp Billing

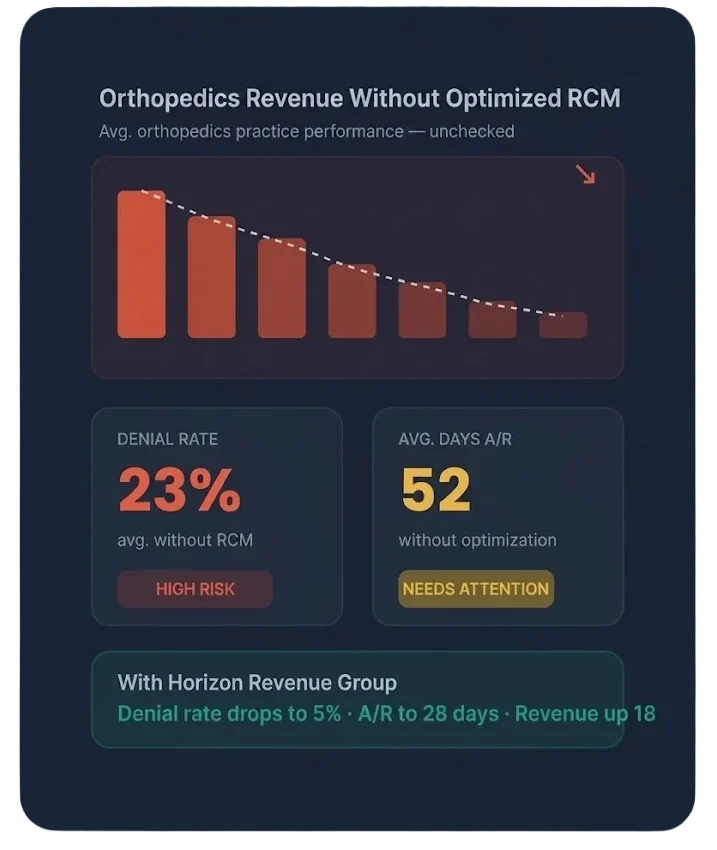
Why Orthopedic Revenue Leaks Are Uniquely Costly
Global Period Billing Errors
Services rendered within the 10- or 90-day global surgical period are routinely denied without proper modifiers. Errors here cost orthopedic practices thousands per surgeon monthly.
Implant & Hardware Revenue Lost
Joint replacement hardware, bone grafts, and spinal implants require precise invoice documentation and HCPCS coding. Generic billers miss pass-through reimbursement on high-cost devices every day.
Modifier & Bundling Mistakes
Incorrect application of modifiers -51, -59, -RT/-LT, -XS, and bilateral procedure rules silently erodes reimbursement across high-volume procedure days — often going undetected for months.
Workers' Comp & No-Fault Complexity
Orthopedic practices treating injured workers face unique fee schedules, jurisdictional billing rules, and adjuster coordination requirements that commercial billing systems are not designed to handle.
Complete Orthopedic RCM Coverage — Zero Gaps
Surgical Prior Authorization
End-to-end prior authorization management for all orthopedic procedures — joint replacements, arthroscopic surgeries, spinal fusions, and fracture repairs — with medical necessity documentation, peer-to-peer coordination, and real-time status tracking before every case.
Musculoskeletal CPT Coding
Certified orthopedic coders assign precise CPT codes across joint replacement, arthroscopy, fracture care, spinal surgery, and soft tissue procedures — capturing the full complexity of each encounter with correct modifier application and bundling compliance.
Implant & Hardware Billing
Comprehensive billing workflows for orthopedic implants, bone grafts, fixation hardware, and spinal devices — including invoice collection, HCPCS coding, claim attachment documentation, and payer-specific pass-through billing to ensure full cost recovery on every high-cost device.
Global Period Management
Expert tracking and management of all 10-day and 90-day global surgical periods — including correct modifier application for unrelated E/M visits, staged procedures, return trips to the OR, and post-operative complications to protect every dollar of post-surgical reimbursement.
Denial Management & Appeals
Rapid denial analysis within 48 hours for all orthopedic claim denials — including bundling denials, medical necessity downcodes, and implant charge rejections. Targeted appeals with operative notes, imaging records, and prior authorization documentation to overturn denials efficiently.
Workers' Comp & No-Fault Billing
Specialized billing for orthopedic Workers' Compensation and no-fault claims — including state-specific fee schedule compliance, adjuster coordination, independent medical examination (IME) billing, and lien management for maximum recovery on injury-related cases.
Provider Credentialing & Enrollment
Complete provider credentialing and payer enrollment for orthopedic surgeons, physician assistants, and NPs — including CAQH management, Medicare/Medicaid enrollment, commercial network contracting, and group practice re-credentialing to eliminate claim rejections from lapsed credentials.
A/R Recovery & Follow-Up
Proactive follow-up on all outstanding orthopedic claims, aged A/R recovery for balances 30–180+ days, and dedicated outreach to commercial payers, Medicare, and Workers' Compensation carriers — recovering revenue your current billing has left on the table.
Orthopedic Analytics & Reporting
Real-time dashboards with procedure-level reimbursement benchmarking, surgeon productivity analysis, payer contract performance, implant cost-versus-reimbursement tracking, and monthly financial reports to drive practice profitability decisions.
— Key Benefits
Measurable Outcomes for Orthopedic Practices
Maximum CPT Reimbursement on Every Case
Orthopedic-credentialed coders ensure every procedure component, add-on code, and modifier is correctly applied — recovering revenue that generic billing companies consistently leave uncollected.
Zero Authorization-Related Surgical Denials
Proactive prior auth tracking, real-time eligibility verification, and clinical documentation support prevent the costly surgical denials that drain orthopedic practices operating without specialized billing oversight.
Full Implant & Hardware Revenue Recovery
Structured implant billing workflows with invoice verification and HCPCS coding ensure that every joint replacement component, spinal implant, and fixation device is fully reimbursed — not written off.
Seamless Workers' Comp & Multi-Payer Coordination
Expert adjudication across commercial insurance, Medicare, Medicaid, Workers' Compensation, and no-fault payers — with jurisdiction-specific billing rules applied correctly for every claim type in your payer mix.
A Structured Workflow Built for Surgical & Clinical Volume
Orthopedic Expertise That Generic Billers Simply Don't Have
COC & Orthopedic-Credentialed Coding Specialists
Our coders hold AAPC Certified Outpatient Coder (COC) and Certified Professional Coder (CPC) credentials with dedicated orthopedic specialty training — covering joint replacement, sports medicine, spine, trauma, and pediatric ortho.
Payer Contract Intelligence for Orthopedic Schedules
We maintain current knowledge of payer-specific orthopedic fee schedules, carve-out arrangements, implant cost limits, and bundling policies — ensuring you collect every dollar of your negotiated reimbursement.
Multi-Payer Expertise Including Workers' Comp
Seamless handling of commercial insurance, Medicare, Medicaid, Workers' Compensation, no-fault, and self-pay billing — with jurisdiction-specific rules applied correctly across all claim types simultaneously.
Ongoing CMS & Regulatory Compliance Monitoring
We proactively monitor CMS fee schedule updates, CPT code changes, AUC compliance requirements, and payer policy shifts — keeping your orthopedic practice compliant and audit-ready at all times.

— FAQs
Orthopedic Billing Questions — Answered
Clear, data-backed answers to the financial questions your CFO cares about most.
— Start Today
