— Certified Medical Billing Services
Medical Billing That Recovers Every Dollar You've Earned
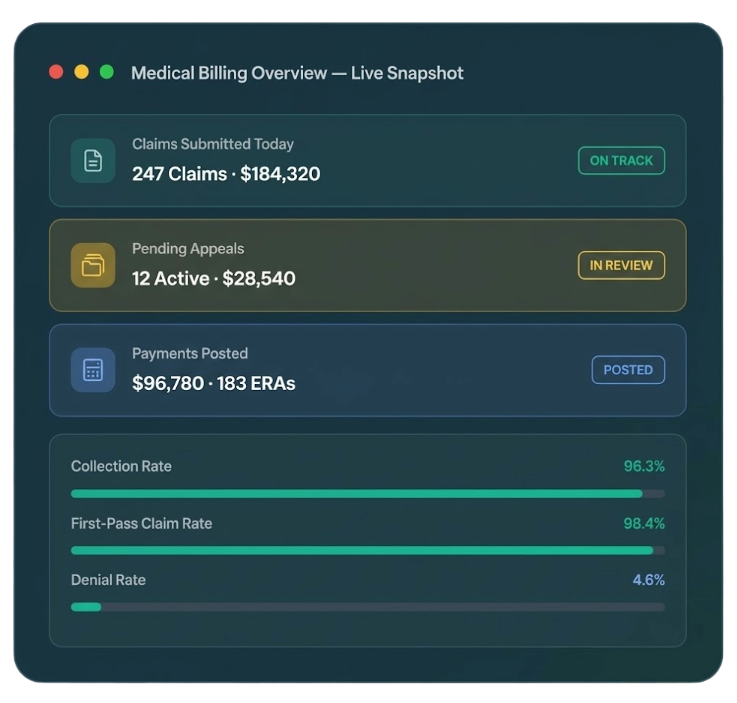
Horizon Revenue Group's certified medical billing team handles claim preparation, payer submission, denial resolution, and patient collections — eliminating revenue leakage and accelerating reimbursements from every major insurer.
HIPAA Compliant
AAPC & AHIMA Certified
Full Cycle Coverage
500+ Practices Served
— What Is Medical Billing
The Financial Engine Behind Every Patient Encounter
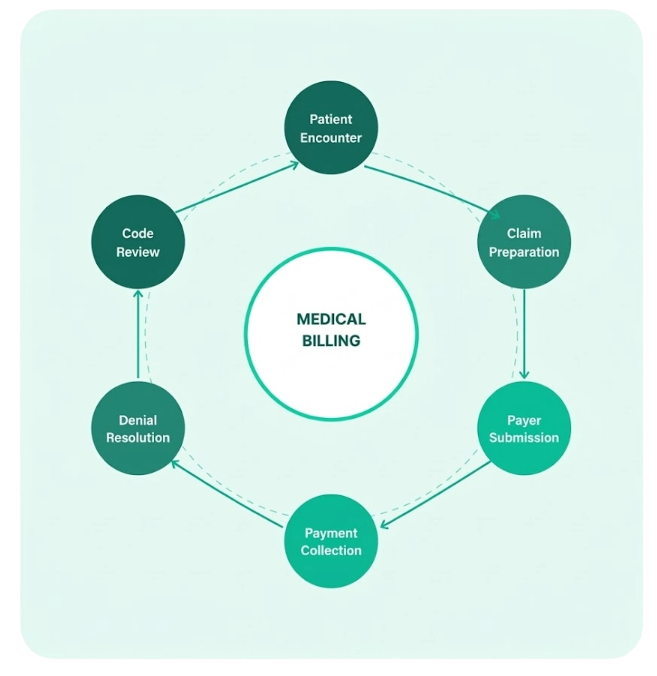
Medical billing is the systematic process of translating clinical services into billable claims and collecting reimbursement from insurance payers and patients. Done right, it's the engine of sustainable practice revenue.
At Horizon Revenue Group, our certified billing specialists handle every step — from encounter documentation review and accurate ICD-10/CPT code assignment to electronic claim submission, real-time payer follow-up, denial appeals, and patient billing. We bridge the gap between clinical care delivery and financial realization, ensuring your practice is paid fully and promptly for the services you provide.
● ICD-10 & CPT Expertise
● All Payer Types
● Government & Commercial
● EHR Agnostic
—Why It Matters
Billing Errors Are Silently Draining Your Practice
Inefficient medical billing is one of the top three causes of revenue loss in healthcare — yet most practices don't track it until it becomes a crisis.
Incorrect or Incomplete Coding
Wrong CPT codes, missing modifiers, and underdocumented diagnoses result in denied claims and lost revenue that is rarely recovered without a systematic appeals process.
Delayed or Missed Claim Submission
Timely filing limits vary by payer. Late submissions mean automatic denials — no appeal possible. Every day of delay increases the risk of unrecoverable revenue.
Unworked Denial Backlogs
Most in-house teams lack the bandwidth to appeal every denial. Stacked, unworked denials directly translate to write-offs that accumulate into significant annual losses.
Payer Rule Changes & Compliance Gaps
Medicare, Medicaid, and commercial payers continuously update billing requirements. Outdated practices lead to compliance issues, claim rejections, and potential audits.

— What's Included
Comprehensive Medical Billing, End to End
Every component of the billing cycle is managed by our team — no handoffs, no gaps, no revenue left uncollected.
Charge Capture & Review
Every service rendered is captured and reconciled against provider notes to ensure no billable encounter is missed, preventing silent revenue loss from day one.
ICD-10 & CPT Code Assignment
AAPC-certified coders apply precise diagnosis and procedure codes with correct modifiers for every encounter — maximizing reimbursement while minimizing audit risk.
Claim Scrubbing & Submission
Claims are validated against 4,500+ payer-specific edits before electronic submission within 24 hours of service — eliminating preventable rejections before they happen.
Insurance Eligibility Verification
Real-time benefits and eligibility checks before every patient encounter confirm active coverage, correct co-pays, and pre-authorization requirements — eliminating front-end denials.
Denial Management & Appeals
Every denial is reviewed and appealed within 48 hours. Root-cause analysis prevents recurrence, and our 94% appeal success rate ensures maximum recovery from disputed claims.
ERA/EOB Payment Posting
Accurate, same-day electronic remittance posting with variance analysis detects underpayments and ensures every dollar collected is reconciled to your practice management system.
A/R Follow-Up & Collections
Proactive follow-up on all open receivables with age-based escalation protocols brings average days in A/R to under 24 days and systematically recovers aged balances.
Patient Billing & Statements
Clear, HIPAA-compliant patient statements with online payment options and automated balance reminders improve patient collections while preserving positive patient relationships.
Billing Analytics & Reporting
Real-time dashboards track KPIs including clean claim rate, denial trends, payer mix, and collections benchmarking — full financial transparency for practice leadership.
— Key Benefits
Quantifiable Results Within Your First 90 Days
Every Horizon medical billing client experiences measurable improvements across all revenue cycle KPIs — tracked and reported with full transparency.
Higher Revenue, Fewer Write-Offs
Certified coders, proactive denial management, and thorough A/R follow-up ensure every legitimate claim is paid — reducing write-offs by an average of 68% within the first quarter.
Reduced Administrative Burden
Free your clinical staff from billing calls, payer portals, and denial paperwork. Horizon absorbs the administrative complexity so your team focuses entirely on patient care.
Faster Cash Flow & Lower Overhead
Same-day claim submission and disciplined A/R management accelerate reimbursements by 40%. Eliminate billing staff salaries, training, and software costs simultaneously.
Continuous Compliance Assurance
Our team monitors CMS updates, payer policy changes, and ICD-10 code revisions in real time — keeping your billing compliant and your practice protected from costly regulatory risk.
— Our Billing Process
A Proven 5-Step Billing Methodology
From onboarding to ongoing billing operations, our structured process is designed for results from week one — with zero disruption to your existing workflows.
— Why Horizon
The Billing Partner Built for Revenue-Focused Practices
Most billing services submit claims and wait. Horizon engineers a billing operation that proactively chases every dollar owed to your practice — every single day.
Certified Specialty Billers, Not Generalists
Every billing specialist holds AAPC or AHIMA certification in your specialty — domain experts who know your payers, codes, and denial patterns intimately.
Performance-Based Fee Structure
We charge a percentage of collections — no flat fee, no setup cost. Our success is tied directly to how much revenue we recover for your practice.
AI-Powered Claim Intelligence
Proprietary claim scrubbing technology and denial prediction models catch errors before submission — ensuring first-pass rates that in-house teams simply cannot match.
Real-Time Transparency, Always
24/7 access to your billing dashboard. See every submitted claim, payment, denial, and KPI trend in real time — no black box, no guessing about your revenue.

We support all major payers including Medicare, Medicaid, Blue Cross Blue Shield, Aetna, Cigna, UnitedHealthcare, and hundreds of regional and commercial insurers. Our certified billers cover 10+ medical specialties including cardiology, internal medicine, dermatology, mental health, orthopedics, pediatrics, ophthalmology, and urgent care.
Yes — Horizon is fully EHR agnostic. We integrate with all major systems including Epic, Athenahealth, eClinicalWorks, Kareo, Modernizing Medicine, DrChrono, and over 50 others. Our onboarding team manages the full integration process with zero disruption to your clinical workflows.
Most practices see measurable improvements within the first 30–60 days — including faster claim submissions, lower denial rates, and improved cash flow. Full results are typically realized within 90 days. During onboarding, we conduct a comprehensive billing audit that often identifies immediate recovery opportunities from your existing denied or aging A/R.
We operate on a percentage-of-collections model — meaning you pay nothing unless we collect. There are no setup fees, no monthly minimums, and no long-term contracts required. Our fee is typically offset within the first month by the revenue recovery and overhead savings we deliver. Contact us for a custom quote based on your specialty, volume, and payer mix.
— FAQs
Common Questions About Our Medical Billing Service
Clear, data-backed answers to the financial questions your CFO cares about most.
— Start Today
Ready to Maximize Your Practice Revenue?
Get a free, no-obligation medical billing audit and discover exactly how much revenue your practice is leaving on the table right now.
