— ASC Billing & Revenue Cycle Management
ASC Billing That Captures Every
Surgical Dollar
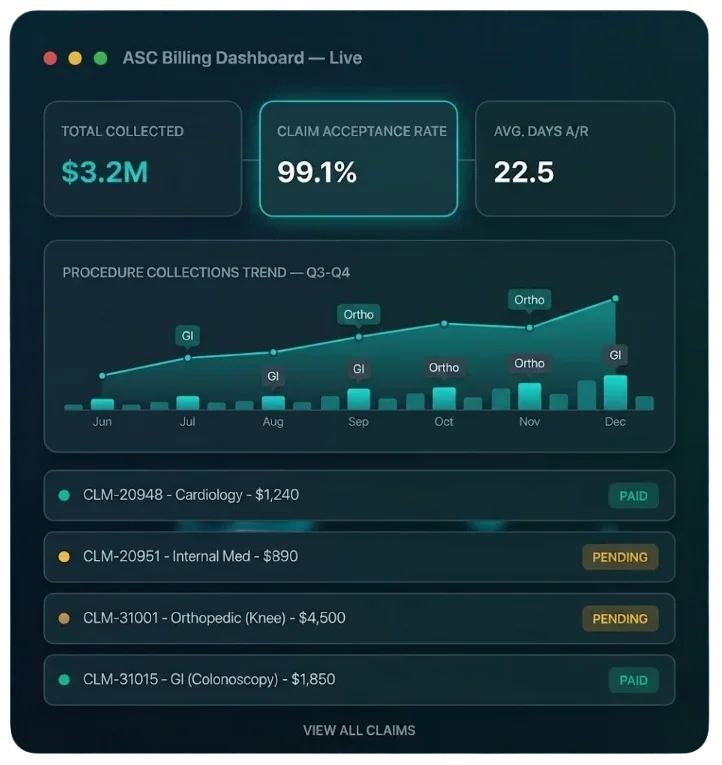
Ambulatory Surgery Centers face uniquely complex billing requirements — facility fees, implant reporting, modifier stacking, and payer-specific reimbursement rules. Horizon Revenue Group specializes in ASC billing to maximize collections and eliminate costly denials.
HIPAA Compliant
ASC-Certified Coders
200+ ASCs Served
24-Hour Case Submission
The Most Complex Billing in Outpatient Healthcare — Handled
Horizon Revenue Group's ASC-specialized billing team brings deep expertise in UB-04 facility claim submission, CMS Ambulatory Payment Classification coding, implant invoice documentation, and payer-specific ASC fee schedule negotiation. We don't apply generic billing practices — we engineer a revenue cycle built specifically for surgical environments.
● UB-04 & CMS-1500
● APC Coding Expertise
● Implant Billing
● Prior Auth Management

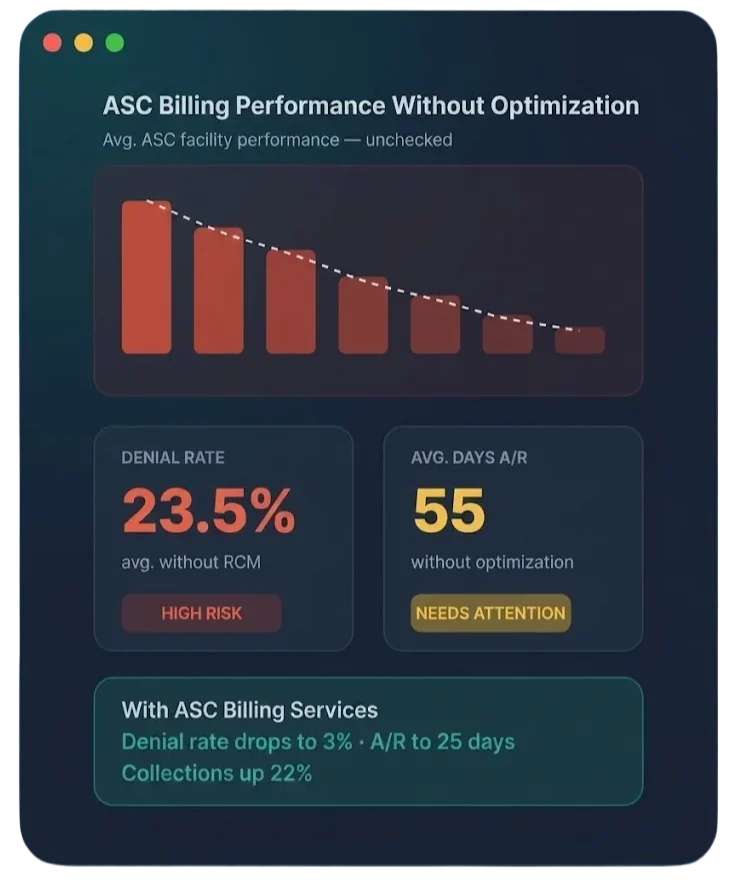
Why ASC Revenue Leaks Are Uniquely Costly
Missing Authorization & Medical Necessity
Surgical procedures without airtight prior authorizations and documented medical necessity result in blanket facility denials — often exceeding $10,000 per case.
Implant & Supply Billing Errors
Implant invoices not properly attached or pass-through charges miscoded leave significant revenue uncollected — especially for orthopedic and spine cases.
APC Grouper & Modifier Mistakes
Incorrectly grouped APCs, missing -73/-74 modifiers for cancelled procedures, and multiple-surgery rule misapplication silently erode your facility reimbursement.
Payer Credentialing Gaps
ASCs operating out-of-network with major payers — or with expired facility credentialing — face recurring claim rejections that delay reimbursement by months.
Complete ASC Billing Coverage — Zero Gaps
Surgical Prior Authorization
End-to-end authorization management for every scheduled case — including peer-to-peer coordination, medical necessity documentation, and real-time status tracking — so your OR never stops due to auth failures.
Facility Fee Coding (APC / HCPCS)
Certified ASC coders assign precise APC groupings, HCPCS Level II codes, and revenue codes on UB-04 claims — capturing the full value of every surgical encounter without unbundling exposure.
Implant & Supply Pass-Through Billing
Comprehensive implant invoice collection, documentation, and claim attachment workflows — ensuring orthopedic hardware, spine implants, and medical devices are fully reimbursed by payers every time.
UB-04 Claim Submission & Scrubbing
Facility claims scrubbed against ASC-specific payer edits — including condition codes, occurrence codes, and value codes — before same-day electronic submission to all major commercial and government payers.
ASC Denial Management & Appeals
Rapid denial review within 48 hours for all facility and professional fee denials. Targeted appeals with operative notes, implant invoices, and authorization records — with payer-specific escalation protocols.
A/R Follow-Up & Collections
Proactive follow-up on all outstanding surgical claims, aged balance recovery for cases 30–120+ days, and coordination with anesthesia and professional billing groups to resolve coordinated claim issues.
ASC Facility Credentialing
Full facility credentialing and re-credentialing with Medicare, Medicaid, and all commercial payers — including CAQH management, payer enrollment, and in-network contract optimization for your specialty mix.
Patient Cost Estimation & Billing
Pre-surgery patient cost estimates, clear post-procedure statements with itemized surgical charges, and online payment portals — improving patient satisfaction and accelerating out-of-pocket collections.
ASC Analytics & Compliance Reporting
Real-time dashboards with case mix analysis, payer reimbursement benchmarking, implant cost-vs-reimbursement reporting, and CMS ASCQR quality reporting support to maintain Medicare certification.
— Key Benefits
Measurable Outcomes for Ambulatory Surgery Centers
Maximized Facility Fee Reimbursement
ASC-specialized coders ensure every facility service line, implant charge, and supply cost is correctly coded and billed — recovering revenue that generic billers consistently miss.
Eliminated Authorization-Related Denials
Proactive prior authorization tracking, medical necessity documentation, and real-time eligibility verification prevent the costly facility claim denials that most ASCs accept as inevitable.
Full Implant & Supply Revenue Capture
Structured implant billing workflows with invoice verification ensure that high-cost orthopedic, spine, and cardiac implants are never left unbilled or underpaid.
Ongoing CMS & Regulatory Compliance
Stay ahead of Medicare Ambulatory Payment Classification updates, ASCQR reporting deadlines, and payer policy changes — with expert guidance built into your billing program.
A Structured Approach Built for Surgical Volume
ASC Expertise That Generic Billing Companies Don't Have
ASC-Credentialed Coding Specialists
Our coders hold AAPC Certified Outpatient Coder (COC) and ASC-specific credentials — with specialty expertise across orthopedics, GI, ophthalmology, pain management, and more.
Dedicated ASC Payer Contract Intelligence
We maintain up-to-date knowledge of payer-specific ASC fee schedules, carve-out arrangements, and contract terms — ensuring you never leave negotiated reimbursement uncollected.
Integrated Facility & Professional Fee Coordination
Seamless coordination between facility billing and surgeon/anesthesia professional billing groups — eliminating cross-claim conflicts and coordinating benefits correctly every time.
CMS Compliance & ASCQR Reporting Support
We monitor CMS regulatory updates, APC weight changes, and ASCQR quality reporting deadlines so your center remains compliant and Medicare-certified without added administrative burden.

— FAQs
ASC Billing Questions — Answered
Clear, data-backed answers to the financial questions your CFO cares about most.
— Start Today
