— Provider Credentialing & Enrollment
Get Credentialed Faster. Bill With Confidence.
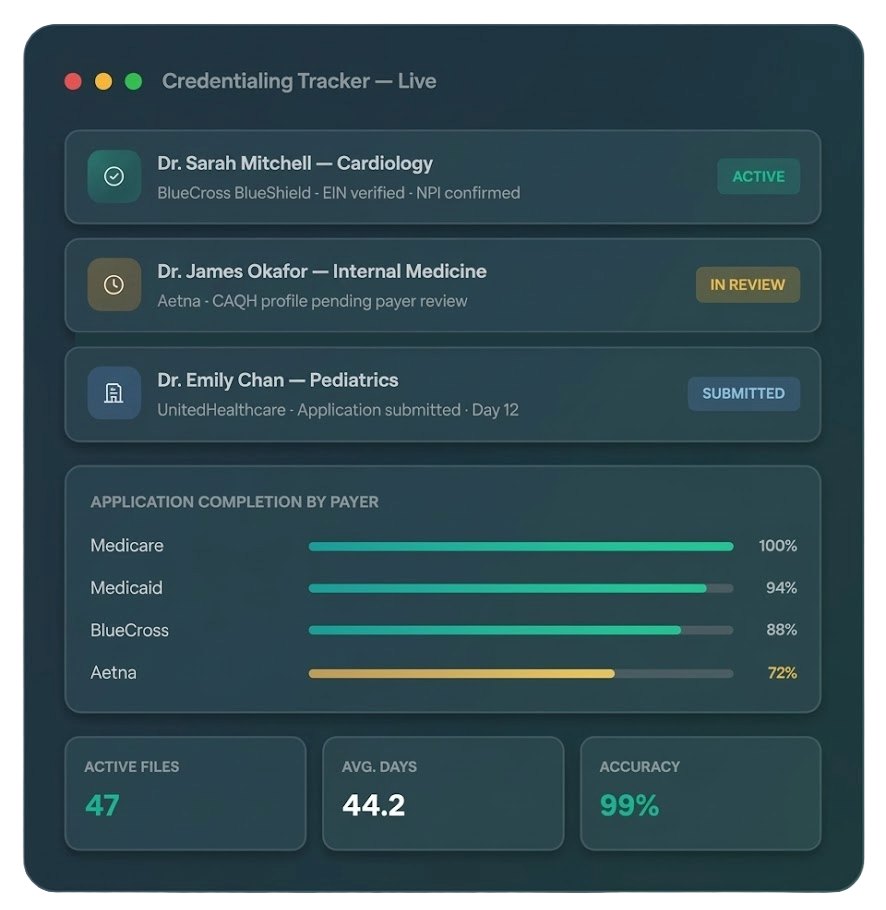
Horizon Revenue Group manages the entire credentialing lifecycle — from initial payer applications to re-credentialing and roster maintenance — so you get in-network faster and never miss a reimbursement window.
HIPAA Compliant
Certified Billers
Full Cycle Coverage
500+ Practices Served
— What Is Credentialing
The Foundation of Your Practice's Revenue Stream
Provider credentialing is the formal verification process by which insurance payers confirm a clinician's qualifications, licensure, training, and professional history before authorizing them to bill for services rendered.
Without active credentialing, your practice cannot bill in-network — meaning every claim is either denied, paid at out-of-network rates, or written off entirely. Horizon's dedicated credentialing team manages every application, follow-up, and renewal across all major payers so your providers are enrolled quickly, accurately, and maintained continuously.
● Initial Enrollment
● Re-credentialing
● CAQH Management
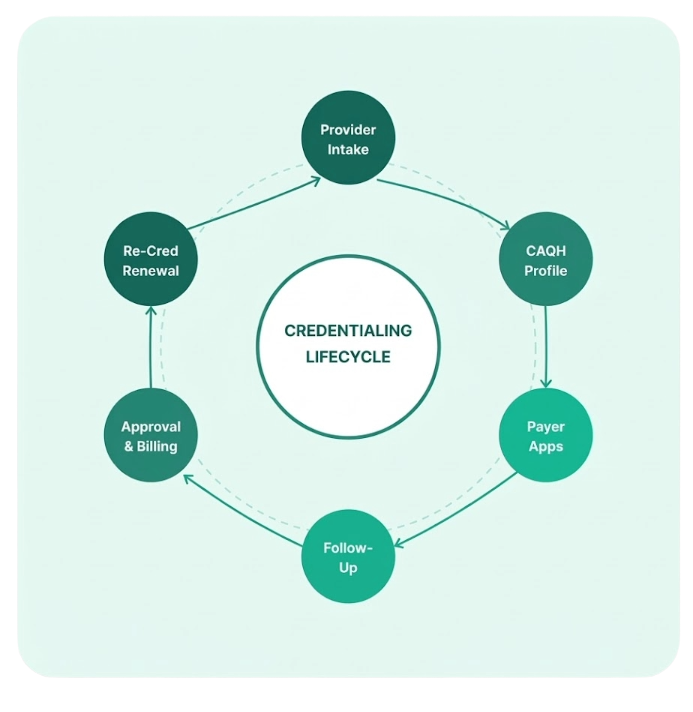
— The Challenge
Credentialing Gaps Are Quietly Costing You Revenue
Unmanaged credentialing creates billing voids, claim denials, and compliance risks that silently drain your practice's financial performance.
Delayed Payer Enrollment
Incomplete applications and missing documentation stall enrollment by weeks or months, leaving providers unable to bill — and revenue unrecoverable.
Lapsed Re-Credentialing
Most payers require renewal every 2–3 years. Missed deadlines result in automatic disenrollment, claims being returned unpaid, and costly re-enrollment backlogs.
CAQH Profile Errors
Outdated or inaccurate CAQH profiles cause automatic rejections across multiple payers simultaneously, triggering widespread billing failures with no visibility into the root cause.
Group vs. Individual Enrollment Confusion
Failing to enroll providers under both individual NPI and group NPI leads to claim rejections that are difficult to trace and expensive to resolve retroactively.

— What's Included
Full-Spectrum Credentialing, End to End
Every credentialing function your practice needs — handled by specialists who do this every single day.
Initial Payer Enrollment
Complete application management with all major commercial payers, Medicare, and Medicaid — including document gathering, form completion, and submission tracking.
CAQH Profile Setup & Maintenance
We create, complete, and attest your CAQH ProView profile on schedule — ensuring your information is always current and preventing downstream payer rejections.
Re-Credentialing & Renewals
Proactive renewal tracking with 90-day advance notice. We manage every re-credentialing cycle so your providers never face a gap in network participation.
Primary Source Verification
Thorough verification of medical licenses, DEA certificates, board certifications, malpractice history, education, and training directly from issuing sources.
Group & Individual NPI Enrollment
Enrollment under both individual and group NPI numbers across all applicable payers, eliminating the split-billing errors that cause silent claim denials.
Medicare & Medicaid Enrollment
End-to-end PECOS enrollment for Medicare and state Medicaid applications — including revalidation management and 855 form completion with audit-ready accuracy.
Payer Follow-Up & Escalation
Persistent status tracking with payer representatives, escalation protocols for delayed applications, and documented follow-up to keep your enrollment on schedule..
Provider Roster Management
Ongoing roster maintenance for group practices and health systems — adding new providers, updating addresses, and reflecting practice changes with payers in real time.
Credentialing Status Reporting
Real-time portal access to all active credentialing files, application status, renewal timelines, and payer correspondence — full visibility for your administrative team.
— Key Benefits
Why Fast, Accurate Credentialing Changes Everything
Efficient credentialing is not just administrative — it is a direct driver of revenue. Every day a provider is unenrolled is a day of revenue lost permanently.
Faster Revenue Start Dates
Our streamlined application process and payer relationships cut enrollment time in half — meaning new providers start billing weeks earlier and revenue gaps are minimized.
Zero Revenue Interruptions from Lapses
Proactive renewal calendars with 90-day lead time mean your practice never experiences the billing shutdowns that come from expired credentialing or missed attestations.
Reduced Administrative Burden
Free your front office and practice managers from credentialing's complexity. Horizon takes ownership of every file, follow-up, and document — you focus on patient care.
Compliance & Audit Readiness
Every credentialing file is documented, timestamped, and retained per regulatory requirements — giving your practice a defensible compliance record at all times.
From Application to Approval — Managed Every Step
Our proven 5-step credentialing methodology is built to minimize delays, eliminate errors, and get your providers billing in-network as quickly as possible.
— Why Choose Horizon
The Strategic Advantage of Expert Credentialing Management
In-house credentialing is slow, error-prone, and consumes staff time that belongs at the front desk. Horizon delivers specialized expertise at a fraction of the cost.
Dedicated Credentialing Specialists
Our team handles credentialing exclusively — not as an afterthought to billing. Deep payer relationships and institutional knowledge accelerate every file.
Real-Time Status Transparency
24/7 access to your credentialing dashboard. See every file, every payer status, every pending action — no waiting for weekly updates or status calls.
Proactive Renewal Management
Automated calendar tracking with 90-day advance notice ensures no re-credentialing deadline is ever missed — protecting your billing rights continuously.
Seamless RCM Integration
When credentialing and billing are managed together, effective dates are tracked accurately, payer IDs are enrolled correctly, and billing starts on day one of approval.

Yes. We manage both individual and group-level enrollments. When a new provider joins your practice, we add them to all existing group payer rosters and initiate any payer-specific individual enrollments required — ensuring they're billing correctly from the earliest possible effective date.
Our team monitors all payer communications and responds to documentation requests within 24 hours. We maintain a complete document library for each provider and coordinate directly with payer representatives — you are notified only if a signature or new document is required from the provider.
Yes. We maintain an active renewal calendar for every provider and every payer in your portfolio. You receive automated alerts 90 days before any expiration — licenses, DEA certificates, malpractice coverage, or payer re-credentialing cycles. We manage all renewals proactively so your billing is never interrupted.
We credential providers across 10+ specialties including internal medicine, family practice, cardiology, orthopedics, dermatology, psychiatry and behavioral health, pediatrics, OB/GYN, radiology, and surgical specialties. Each specialty has unique payer requirements — our specialists have deep experience navigating them all.
— FAQs
Credentialing Questions, Answered Clearly
Clear, data-backed answers to the financial questions your CFO cares about most.
— Start Today
Get Your Providers Credentialed Faster
Speak with a credentialing specialist today. We'll review your current enrollments and identify opportunities to accelerate approvals and close any coverage gaps.
