— End-to-End Revenue Cycle Management
Maximize Every Dollar You've Earned
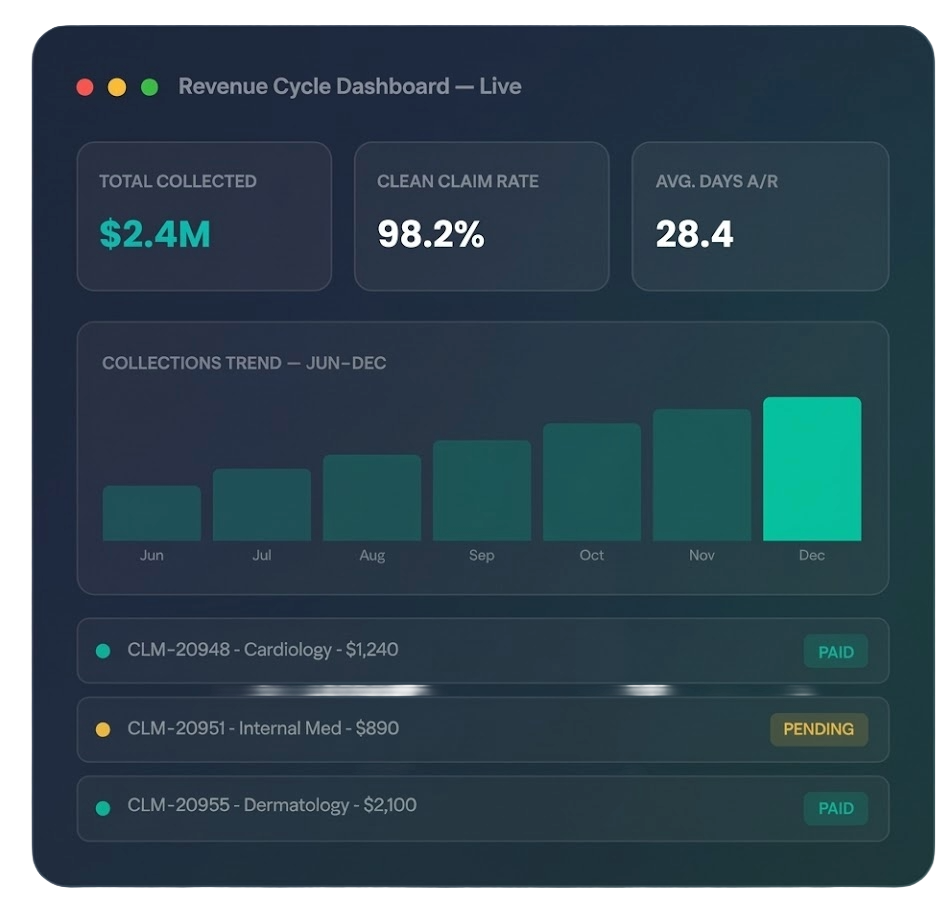
Horizon Revenue Group manages your entire billing cycle — from eligibility verification to final payment — reducing denials, accelerating reimbursements, and delivering full financial visibility.
HIPAA Compliant
Certified Billers
Full Cycle Coverage
500+ Practices Served
— What We Do
Your Practice's Complete Revenue Cycle — Managed
RCM is the financial heartbeat of your practice. Horizon handles every step — from pre-visit eligibility verification to final payment reconciliation — so your team focuses on patients, not paperwork.
Our certified billing specialists bring deep specialty expertise across cardiology, internal medicine, dermatology, mental health, pediatrics, and more. We don't just submit claims — we engineer a system that maximizes every legitimate reimbursement, every time.
● End-to-End Coverage
● HIPAA Compliant
● 24hr Turnaround
● Real-Time Dashboards
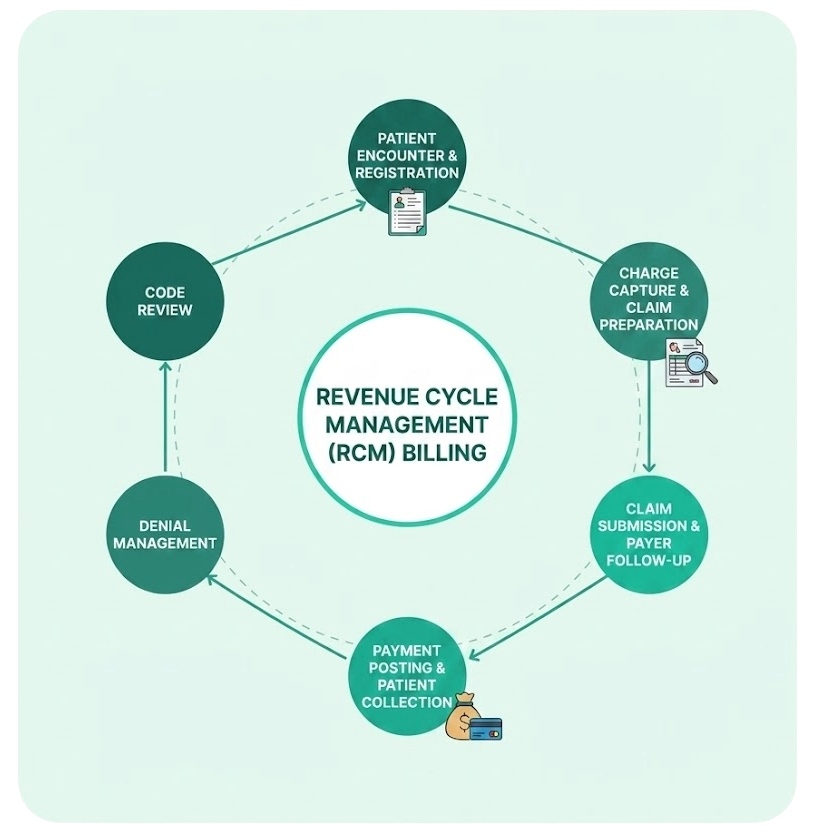
— Why It Matters
End-to-End Revenue Cycle Management, Built for Growth
We manage every stage of your billing lifecycle — from eligibility to payment — so you can focus entirely on patient care.
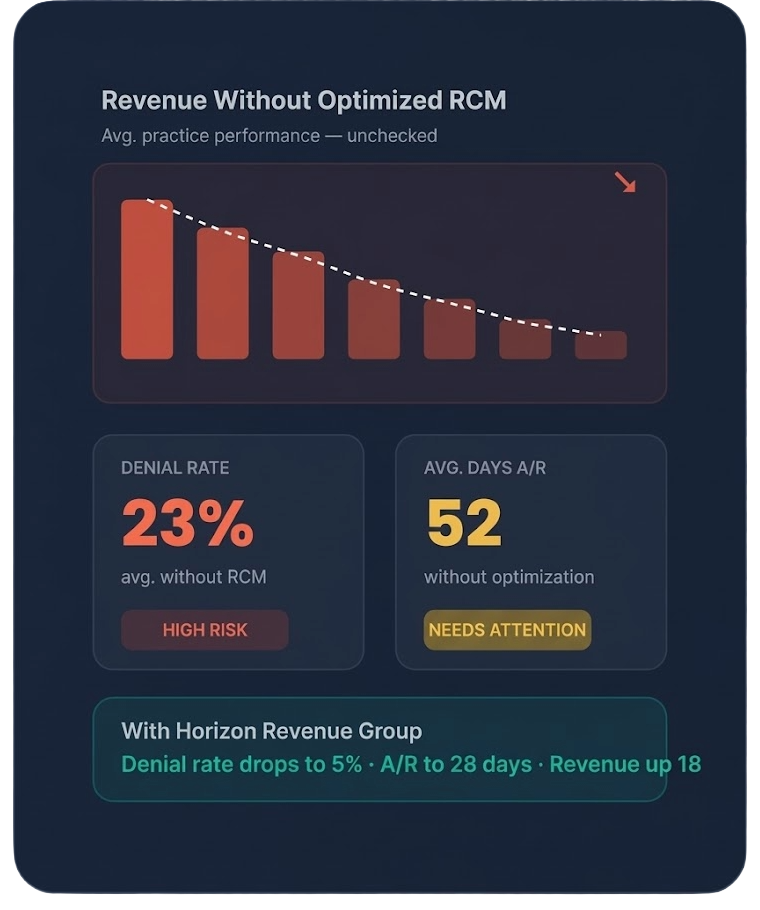
High Claim Denial Rates
Coding errors, missing documentation, and eligibility mismatches directly reduce collections and burden staff with rework cycles.
Slow Reimbursements
Extended days in A/R constrain cash flow, limiting hiring capacity, operational growth, and long-term financial stability.
Coding Errors & Under-Billing
Incorrect CPT codes and missed modifiers silently erode revenue — often thousands per month with no visibility into the problem.
Overwhelmed In-House Teams
Staff spending hours on payer follow-up and appeals means less time for patient experience and clinical coordination.
— Services Included
Every Part of Your Billing Cycle, Covered
A fully managed RCM suite — no gaps in coverage, no billing functions left unmanaged.
Patient Registration & Eligibility
Real-time insurance eligibility verification before every visit eliminates surprise denials and ensures accurate co-pay collection at point of service.
Medical Coding (ICD-10 / CPT)
Certified coders review every encounter, capturing all billable services with correct modifiers to maximize legitimate reimbursement and minimize audit risk.
Claim Submission & Scrubbing
Claims scrubbed against 4,500+ edits before submission, eliminating preventable errors and ensuring electronic delivery within 24 hours of service.
Payment Posting & Reconciliation
Accurate, same-day ERA and EOB posting with variance analysis to catch underpayments and ensure every collected dollar is accounted for.
Denial Management & Appeals
Every denial worked within 48 hours with a targeted appeal strategy. Root cause tracking prevents recurrence and systematically improves your clean claim rate.
A/R Follow-Up & Collections
Proactive payer follow-up on all outstanding claims with age-based escalation protocols to dramatically reduce days in A/R and recover aged balances.
Provider Credentialing
Full credentialing and re-credentialing with all major payers, with managed timelines and status tracking so you never miss a network participation window.
Patient Billing & Statements
Clear, compliant patient statements with online payment portals, balance-due reminders, and a compassionate approach that preserves patient relationships.
Analytics & Reporting
Real-time KPI dashboards with payer mix analysis, denial trending, and collections benchmarking — full financial visibility for your leadership team.
— Key Benefits
Measurable Results That Define Our Standard
Our clients see quantifiable improvements across every revenue cycle metric within the first 90 days of onboarding.
Increased Collections Rate
Clients average 18% more collections than in-house billing — driven by fewer denials, faster follow-up, and complete charge capture on every encounter.
Reduced Overhead Costs
Eliminate salaries, benefits, training, and software costs for in-house billing staff. Horizon delivers expert billing at a fraction of in-house cost.
Accelerated Cash Flow
Same-day claim submission and proactive A/R management means most clients see reimbursements 40% faster after onboarding with Horizon.
Full HIPAA Compliance — Always
HIPAA-trained staff, encrypted data handling, BAA agreements, and regular compliance audits protect your practice.
A Structured Path to Revenue Optimization
Our proven 5-step methodology delivers measurable results from week one — with zero disruption to your existing workflow.
— Why Choose Horizon
The Strategic Advantage Over In-House Billing
In-house billing teams cost more, know less, and produce inferior results. Here is the evidence-based comparison.
Specialty-Certified Billing Experts
Our coders hold AAPC and AHIMA certifications across 10+ medical specialties — domain experts, not generalists.
Transparent, Real-Time Reporting
24/7 access to your revenue cycle dashboard. No black box — every metric and trend visible to your team at all times.
Technology-Driven, Human-Executed
AI-powered claim scrubbing and denial prediction — backed by experienced billers who manage every exception personally.
Dedicated Account Management
A named account manager who knows your practice, your payers, and your goals — available by phone or email, always responsive.

We operate on a percentage-of-collections model — no flat monthly fee, no hidden setup charges. You only pay when we collect. This aligns our incentives directly with your revenue growth. Contact us for a custom quote based on your specialty and volume.
Every denial is reviewed within 48 hours. Our team identifies root causes, prepares targeted appeals with supporting documentation, and tracks each through resolution. We report denial trends monthly so you can see systemic improvements over time.
Absolutely. Horizon Revenue Group is fully HIPAA compliant and executes a Business Associate Agreement (BAA) with every client. Staff undergo annual HIPAA training, all data is encrypted in transit and at rest, and we conduct regular compliance audits.
You get real-time access to a personalized analytics dashboard showing clean claim rate, days in A/R, denial rate, collections by payer, and more. Monthly executive summaries and quarterly business reviews with your account manager provide strategic insight, not just raw numbers.
— FAQs
Answers to Questions Your CFO Will Ask
Clear, data-backed answers to the financial questions your CFO cares about most.
— Start Today
Ready to Maximize Your Practice Revenue?
Get a free, no-obligation revenue audit and discover exactly how much your practice could recover.
